




Cancer Care
A Cutting-Edge Tool in the Fight Against Cancer
Published: Nov. 25, 2019
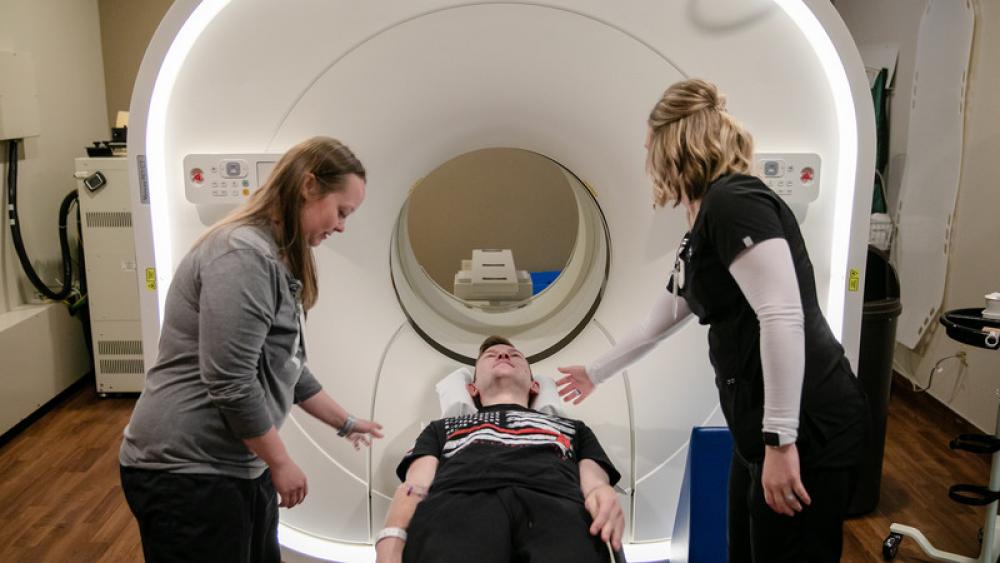
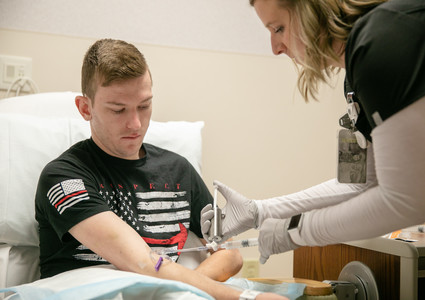
Jake Arnold had been making the trip to Methodist Hospital for five years. Every six months, he’d drive from his home in Villisca, Iowa, and then from his apartment in Bellevue.
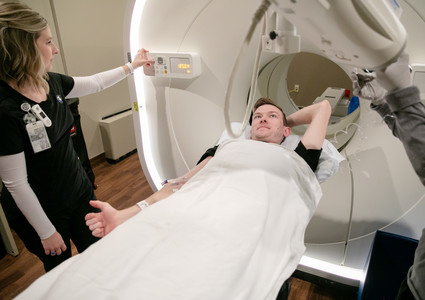
He’d be injected with a radioactive tracer and wait about an hour as it traveled through his body. Then he’d climb onto a table, lie down and relax as a multimillion-dollar positron emission tomography (PET) machine slowly scanned his body, looking for signs that his melanoma may have returned.
The 23-year-old’s skin cancer was in remission, and he’d had 10 PET scans come back clean. On a warm day last April, he hoped No. 11 would, too. He knew another scan with no unusual activity might lead doctors to recommend less frequent visits – the next step on the road to beating cancer.

Jake spent his childhood in Southern California before moving to Iowa in fifth grade. Being outside without sunscreen was the norm, even when he took a lifeguard job in Villisca.
“I was always in the sun. I was always going,” he said. “Summertime, I’d always be out. I’d never wear a shirt.”
He had plans to join the Army after high school. But everything changed at the military entrance processing station. A doctor spotted a suspicious mole on Jake’s back. Testing confirmed it was melanoma that had spread from his back to the lymph nodes under his arms.
At age 17, Jake was a high school senior and a cancer patient. The five-year survival rate for stage 3 patients like him is 64%.
His reaction?
“Disbelief,” he said. “I didn’t know what was going on. My mom told me before school one day. I still went to school fine. But once you start seeing the doctors, everything just hits you, like, ‘Wow, this is real.’”
An Aggressive Plan
Jake’s care team at Methodist included surgeon George Dittrick, MD, who led the team that removed his lymph nodes, and Ralph Hauke, MD, FACP, an oncologist with Nebraska Cancer Specialists. They didn’t sugarcoat things, but they had an aggressive plan.
“They said, ‘You’ll kind of feel like crap, but we’re going to make sure you’re going to be all right,’” Jake said.
After surgery to remove the lymph nodes, Jake underwent immunotherapy at Methodist Estabrook Cancer Center. He’d stay in a nearby hotel Monday-Friday while getting high doses of a cancer-fighting drug, then return home to Iowa on the weekends. After a month of treatments in Omaha, he returned home for good, giving himself a smaller dose of the drug three nights a week.
Two months before his 19th birthday, Jake had his final treatment. The treatments zapped his energy, but they had done their job – there was no longer any evidence of the disease. Now the goal was to keep it that way, and state-of-the-art technology would play a big part.
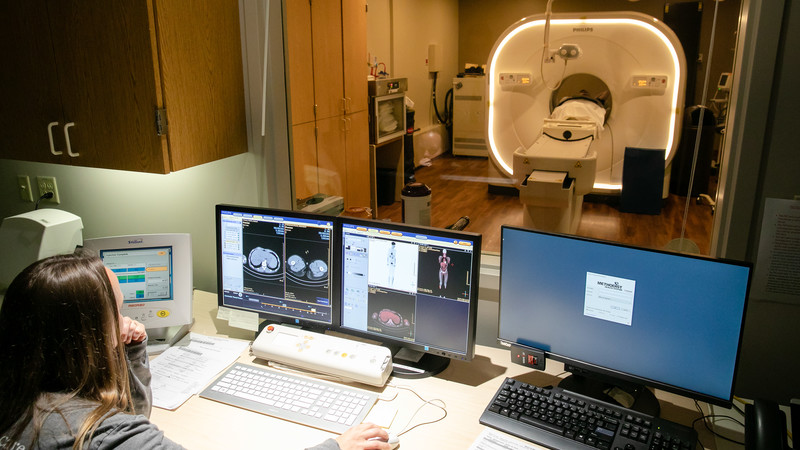
Since 2005, PET scan technology has been an important cancer-fighting tool for Methodist. It involves two scans performed by one machine. First up is a computer tomography (CT) scan that maps a patient’s bone and tissue – essentially a three-dimensional X-ray. That image is fused with the PET scan, which detects a radioactive tracer containing sugar that is injected into patients. The goal is to spot any buildup of the tracer in cancerous tumors, which are highly metabolic and need plenty of energy to grow. A radiologist reviews the image first, then forwards it to the patient’s oncologist to decide the next step in treatment.
As PET scanners have evolved from analog to more precise digital technology, Methodist has responded. Methodist Hospital installed the region’s only digital PET scanner in 2018. The benefits were immediately obvious.
“The three major improvements are decreased scan time, decreased radiation dose to the patient and increased sensitivity of the scanner, which can potentially pick up things earlier,” said Ryan Dvorak, MD, a radiologist at Methodist Hospital.
“I think that’s a big deal, particularly for patients who are going to be long-term survivors,” Dr. Hauke said. “When we’re scanning these folks every three to six months for several years, that’s not a trivial amount of radiation.”
But for Jake, who has endured hours of scans in both machines, one advantage stands out.
“It’s faster,” he said without hesitation. “The reason why it’s better is it’s faster.”
While a CT scan takes only a couple of minutes, an analog PET scan might take about 45 minutes or more and require the patient to turn around on the table to capture their entire body. That time is cut in half with a digital scan, and no patient adjustments are necessary. That means less discomfort for patients and the ability to schedule more scans, giving more people access to this cutting-edge technology.

Jake had a positive attitude going into his scan last spring. He’d had five years of clean scans. He was looking toward his future and a big goal – becoming a professional firefighter. But he always wondered: Will it come back?
Jake had his scan and went home to Bellevue for lunch. He returned to the Methodist Hospital campus that afternoon to meet with Dr. Hauke. The news he delivered was even better than Jake hoped for.
Dr. Hauke told him he needed to see his primary care provider annually and get checked by a dermatologist every six months. As for the scans: They were done.
It was a bittersweet moment for Jake. Through surgery, therapy, scans and checkups, he had spent years getting to know the staff at Methodist Hospital and Methodist Estabrook Cancer Center. They had become friends, and the feeling was mutual.
“I always tell a patient, I’ll be happy to see you in a coffee shop somewhere, but I don’t want to see you back here if I don’t have to,” Dr. Hauke said.
More than anything, Jake had a sense of relief. He was finally moving on from cancer. He’s since had a birthday and a dermatology exam that found nothing. His relief and optimism have only grown.
“It just feels like there’s not a sword above your head,” he said. “I’m not worried about it anymore.”
Photos by Daniel Johnson.
More Resources
- Learn more about cancer care at Methodist.
- Read more from the Winter 2019 issue of The Meaning of Care Magazine


