




Cancer Care
With Recognition Comes Hope in Treating a 'Real Jerk of a Cancer'
Published: March 16, 2020

In August 2018, Tim Echternach and his wife, Keri, took a trip out of town. Keri was on break from nursing school at Nebraska Methodist College, so the couple planned a short getaway. Tim remembers showering in the hotel bathroom and being somewhat alarmed by what he saw.
“I was looking at myself in the mirror,” he said. “All the walls were white. I couldn’t help but notice how yellow I looked in comparison. I called for my wife – who just wrapped up her oncology rotation – and right away, she said, ‘You look jaundiced.’”
It was the final straw for Tim, who decided to make an appointment with his doctor after also suffering from sporadic stomach pain for most of the summer.
“Kind of like heartburn,” he said. “Like, ‘OK, I just ate a big greasy burger, and now I’m paying for it.’ I figured it was some kind of intolerance.”
But his doctor told him it was likely much more serious.
A “Nightmare” Diagnosis
A CT scan and ultrasound revealed a highly concerning mass. A tumor at the head of his pancreas was blocking his bile duct. His eventual diagnosis? Pancreatic adenocarcinoma – or pancreatic cancer.

Tim was referred to Methodist Estabrook Cancer Center (MECC). He needed six cycles of chemotherapy before undergoing surgery – the Whipple procedure – with Methodist surgical oncologist George Dittrick, MD.
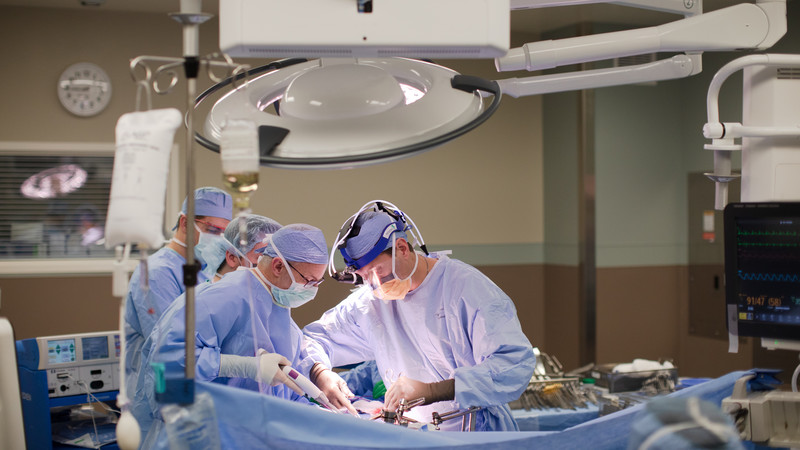
According to Dr. Dittrick, Whipple surgery is a “two-part operation designed to remove the head of the pancreas and all the surrounding tissues to which the cancer is most likely to spread – then reconstruct what’s been removed so that the stomach, bile duct and remaining pancreas all have ways of communicating with the intestinal tract.”
The procedure removed all visible and radiographic evidence of the tumor, but Tim received six more cycles of chemotherapy and a combination of 30 radiation treatments with oral chemotherapy to ensure the best chance of wiping out any cancerous cells that might still be present.
“It was rough,” he said.
But he had no further evidence of disease.
“I gave my wife a hug and a kiss. Through some tears, she said, ‘You did it.’”
Led to the Best
Tim, who’s lived with epilepsy for most of his life and survived a bad motorcycle accident when he was younger, has met his fair share of medical professionals. But cancer led him to some of the best, he said.
“The care I got with Dr. Dittrick and whoever was at the end of my Methodist bed seemed so much more collaborative than anywhere I’ve ever experienced. Everything seemed so personalized. And when nurse after nurse learned that my surgeon was Dr. Dittrick, they all reassured me of his expertise.”
Tim paused.
He apologized for getting emotional.
The five-year survival rate for pancreatic cancer is about 9%, “and they tell you that Whipple has a five-year survival rate of 20%,” Tim said.
He continued: “To hear over and over again that if there’s one surgeon in town or one surgeon in the Midwest to do this procedure, he’s the guy to have, and you’ve got him? Well, I can’t describe what that did for me.”
But Dr. Dittrick acknowledges the entire health system when it comes to treating patients like Tim.
“Yes, it’s better to have one surgeon doing certain procedures 20 or 30 times a year rather than 20 or 30 surgeons doing them once a year,” Dr. Dittrick said. “But it’s just as important to have a health system that knows how to care for patients before, during and after surgery. High-volume facilities that routinely care for patients fighting pancreatic cancer are every bit as important as high-volume surgeons.”
It’s that kind of multidisciplinary approach that landed MECC a National Pancreas Foundation (NPF) Cancer Center designation. It’s the only center in Nebraska and Iowa and one of 50+ highly-esteemed centers nationwide to receive such recognition.
“It’s a notable commendation for the quality and facets of care available here,” Dr. Dittrick said. “And for patients, hopefully it serves as reassurance that there’s somewhere out there that’s seen this problem before, deals with it a lot and considers the most individualized care options available in order to provide the best possible outcomes.”
The Importance of Clinical Trials
Of all the criteria NPF centers must meet, Dr. Dittrick believes one of the most important is the presence of clinical trials.
“Surgeries can only get so safe and technically advanced,” he said. “And compared to other more common types of cancer – like colon or breast – we have so far to go in terms of survival rates. The only way to improve that is by discovering new and better treatments.”
Thomas Millsap, 46, agrees.
He was diagnosed with stage 4 pancreatic and liver cancer in May 2017 and was given six to nine months to live. But with the help of David Silverberg, MD, FACEP, an oncologist with Nebraska Cancer Specialists, and Marlene Watson, RN, BN, OCN, an oncology research nurse navigator with MECC, Thomas was enrolled in a double-blind chemotherapy study managed by Hoosier Cancer Research Network. He’s been in remission for almost three years.

“This is why we do what we do,” Watson said.
“I’m a testament,” Thomas added. “Whatever they’re doing – whatever research is being conducted – it’s working. I mean, stage 4. And now remission. If that doesn’t give someone else hope, I don’t know what will.”
Beating the Odds, Deeming Each Day a Victory
Tim, too, continues beating the odds. He’s more than a year out from surgery and, as far as his doctors can tell, he’s still disease-free.

No matter how many years pass, though, Thomas isn’t sure he’ll ever really feel “in the clear.” And Tim isn’t sure he’ll ever lose his constant “scanxiety” – or fear of CT scans. But both survivors view their days a little differently now.
“I count Christmases,” Thomas said. “It’s my wife’s favorite holiday. And she’s been my rock. I survived three Christmases since my diagnosis.”
“I never was a morning person,” Tim said. “But I’ll tell you what: I rarely miss a sunrise now.”

Photos and video by Daniel Johnson
More Resources
- Learn more about cancer care at Methodist
- Read another man’s story of pancreatic cancer survival at Methodist
- Read more from the Spring 2020 issue of The Meaning of Care Magazine


