
The Meaning of Care Magazine
A markless approach: ‘Utilizing the most advanced technology to save lives and change them for the better’
Published: March 26, 2024
Cancer has an ugly way of leaving its mental or emotional mark on patients.
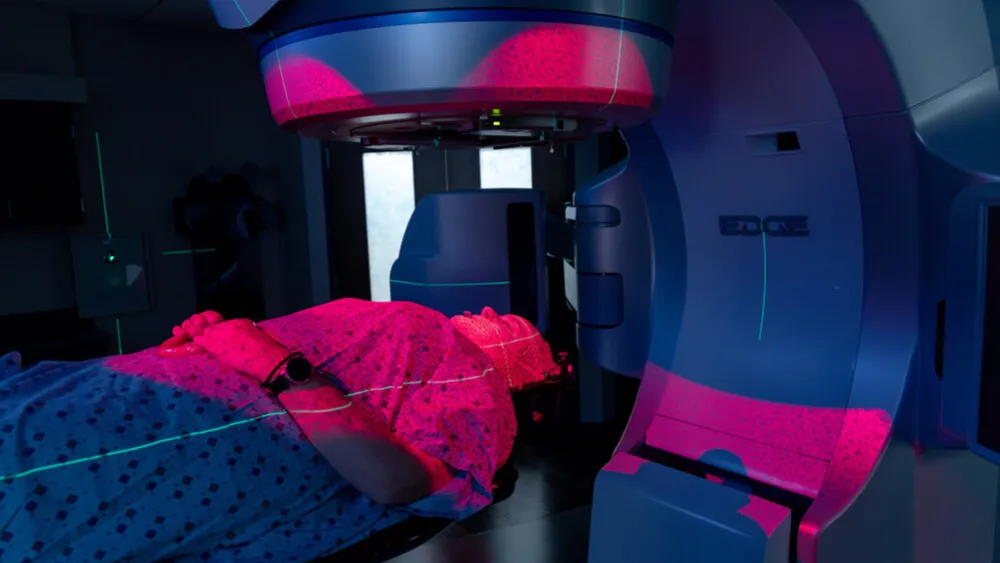
And when it comes to treatment, radiation therapy – which uses intense beams of energy to destroy cancer cells – has often left physical marks on patients, temporarily or permanently.
For years, either freckle-sized tattoos or permanent marker-drawn X’s covered by clear stickers have allowed radiation oncologists and therapists to accurately target a tumor’s location during treatment sessions. Because those sessions are generally multiple days a week for several weeks at a time, it’s important that radiation beams are hitting the same spot every time while minimizing exposure to surrounding healthy tissue.
Preserving quality of life
What sounds like a foolproof method of zeroing in on a tumor, however, isn’t as perfect as it could be.
“Sure, we can do the perfect setup, but there’s always that chance for some variation,” said Methodist radiation oncologist Ming-yang Hung, MD. “Maybe the patient is breathing differently that day, maybe their positioning is slightly off, or they have more gas in their stomach. All these things can affect where the tumor sits in their body. So, you mark a 1- to 2-centimeter margin of healthy tissue around that tumor to account for those variations – just to make sure you’re always hitting the mark.”
But 1 to 2 centimeters is plenty of healthy tissue to mess with.

“Take the brain, for example,” said John Mullins, Methodist Health System’s chief radiation physicist. “Everything that’s not cancer in the brain is obviously very important. You’re talking about potentially damaging regions that control speech, balance, heartbeat and movement. So every bit of healthy brain needs to be protected from radiation. When you’re dealing with the lungs, you worry about a cough developing or breathing issues. Gastrointestinal cancer? You’re looking at potential bowel issues – like urgency or diarrhea, nausea, or stomach bleeding.”
Sometimes more damaging to a patient, though, is a physical reminder – via tattoo or sticker – of what they’re up against and what it’s taking away from them.
“These patients should be able to wear what they want to wear without these marks showing, and they shouldn’t have to explain to their kids or grandkids that these marks are what we use to line them up in a big, scary machine,” said Brandon Crow, a radiation therapist at Methodist Estabrook Cancer Center. “And with the stickers, it’s important that those stay put until treatment is complete. We’ll often have to tell patients, ‘Sorry, you won’t be able to do your daily swim.’ ‘You’re not going to be able to enjoy your hot tub for a while.’ Or, ‘That gardening you like to do makes you sweat too much. You’ll have to cut back on that.’ You can see it in their face – this look of … nothing – when the one thing that might help take their mind off all of this is suddenly off-limits.”
Going markless

Methodist adopted surface-guided imaging – or markless radiation – in 2017. But it wasn’t until a couple years ago that staff really leaned into more training opportunities, which opened it up to more patients.
Thanks to the team’s all-in approach, more patients are now able to experience treatment without being drawn on or tattooed by their radiation therapist.
“It’s not like going to the tattoo parlor – it really is a small dot,” Crow said. “But it is a needle and ink, and it’s permanent. To have the option of not going through that is a benefit in itself.”
Breast, lung as well as head and neck cancer patients now make up a large majority of candidates benefitting from the technology at Methodist, which uses three different cameras to capture specific contours of a patient’s body and keep watch for variation in real time during treatment. This ensures the most precise radiation delivery possible.
“Now, my margin of healthy tissue around the cancer is more like 7 millimeters, which is a lot less than 2 centimeters,” Dr. Hung said. “And even if that smaller margin only eliminated a cosmetic change to the skin, that’s still a quality-of-life issue that was spared because of this technology.”
Before this technology, variation in patient positioning – maybe due to a cough or spasm during treatment – would require the radiation oncology team to stop treatment, enter the treatment room and reposition the patient manually, potentially adding up to five minutes to the treatment session.
“That doesn’t sound like a lot,” Mullins said. “But if you’re nervous, scared, undressed on a cold, hard table, lying in an uncomfortable position, maybe in a mask and you’re claustrophobic, five minutes is an eternity. This technology not only helps ensure accuracy. It also helps ensure the best care and experience possible for the patient.”
Expanding to save, change lives
Because of the positive experiences and successful outcomes that patients continue having with markless radiation, Methodist plans to expand the technology across the health system. Although it’s not the best option for every patient – it’s certainly another innovative approach that reinforces Methodist as a true leader in cancer care.
“I hear from our patients all the time that we’re the best,” Crow said. “I want to keep that going. I want to keep moving forward. And I’m confident we will – by utilizing the most advanced technology to save lives and change them for the better.”
Photos by Dan Johnson
More Resources
- Read more from the spring/summer 2024 issue of The Meaning of Care Magazine.
- Learn more about radiation oncology services at Methodist.
- Learn more about cancer care at Methodist.


