Family Health
Myth-Busting Ear Infections

February is often a rough month for parents when it comes to their children's health. Cold weather and snow typically abound, which combines with cold and flu season to make a rough mix of snotty, cabin-fever kids (at least at my house).
Given that my son has yet another ear infection added to the mix of February's delight, and that this month is Pediatric ENT Month, it seems fitting to talk facts and myths about one of every parent's fears: ear infections.
Ear infection myths and facts
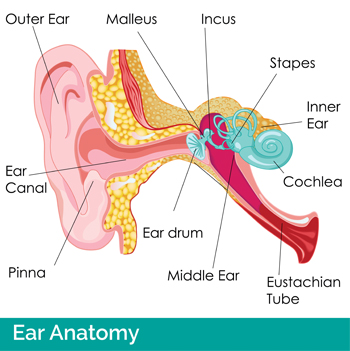 Fact: An ear infection (also called otitis media) is an infection of the middle ear space of the ear and can be caused by both viruses and bacteria.
Fact: An ear infection (also called otitis media) is an infection of the middle ear space of the ear and can be caused by both viruses and bacteria.
The area behind the ear drum becomes infected and full of fluid because the Eustachian tube is not functioning normally. The Eustachian tube is the natural tube we have from our ear to our throat; it’s what pops open on air planes to even pressure between the inside and outside of our ear.
An ear infection is diagnosed by looking at both the appearance and the movement of the ear drum. Signs and symptoms of an ear infection can be fever (temperature above 100.4F), pulling or tugging on the ears, ear drainage, increased fussiness, poor sleep, decrease in appetite and vomiting.
Myth: All ear infections need antibiotics.
Most ear infections are caused by common cold viruses and will improve on their own without antibiotic medication. Most ear infections caused by bacteria will also improve on their own within two or three days. Whether or not a child requires antibiotics depends on their age, history, risk factors and exam. This is why your doctor cannot diagnose an ear infection over the phone.
Fact: Most ear infections occur with or after a cold.
While ear infections can certainly happen on their own, they often come with or on the tail end of a cold that has created swelling, inflammation and increased mucus with a child’s ears, nose and throat.
Myth: An ear infection is an emergency.
In addition to most ear infections resolving on their own, there is very little risk for long-term hearing damage or complications from ear infections. Assuming your child is still breathing comfortably, alert and staying hydrated, they can typically wait until the next day to see a doctor. (Symptoms inevitably show up in the middle of the night- at least in my house). Fever and pain can certainly be treated with Acetaminophen or Ibuprofen to keep kids happy and comfortable.
 Fact: Children in daycare, who are exposed to any cigarette smoke, and who use a nighttime bottle or have a bottle propped are more likely to get an ear infection.
Fact: Children in daycare, who are exposed to any cigarette smoke, and who use a nighttime bottle or have a bottle propped are more likely to get an ear infection.
Being in daycare exposes children to a greater number of colds. Cigarette smoke, in addition to being bad for a child’s lungs, also irritates and inflames the upper airway. Children who eat lying flat on their back (with a bottle propped or overnight) have more fluid in the back of their throat which can enter into the middle ear.
Myth: Water and earwax can cause ear infections.
Assuming a child is otherwise healthy, water in the ear cannot get past the ear drum and cause an ear infection. If water does cause an infection, it is instead an external ear infection (also called swimmers ear) that presents with pain, a foul smell and discharge from the ear. This is because the ear canal gets infected from the water (usually a pool or lake).
Earwax is normal for children to have and helps protect the delicate ear canal. Parents should not clean into their child’s ear canals. In fact, the normal amounts of water children get in their ears with showers and baths keeps earwax soft and functioning normally.
If you have more questions about ear infections, talk with your child’s Methodist Physicians Clinic primary care provider.


