Today's Medicine
Former Smoker Credits Low-Dose CT Scan, Methodist Lung Cancer Program With Saving Her Life
Published: April 9, 2021

Joellen Coon, RT (R)(M), has seen the devastating effects of lung cancer up close.
In 2008, her sister-in-law went to the doctor for a persistent cough and chest pain. She was diagnosed with lung cancer, which spread to her bones.
“She lived two years and passed away. And it was a hard two years with chemo and radiation,” said Joellen, a radiologic technologist and mammographer with Methodist Physicians Clinic. “She had part of her lung removed, and it just never helped.”
Fast forward to last fall, and Joellen, 59, was making changes to improve her health. A smoker for 43 years, she quit in September. She also scheduled a regular checkup around that time with Methodist Physicians Clinic internal medicine physician Andy Welstead, DO.
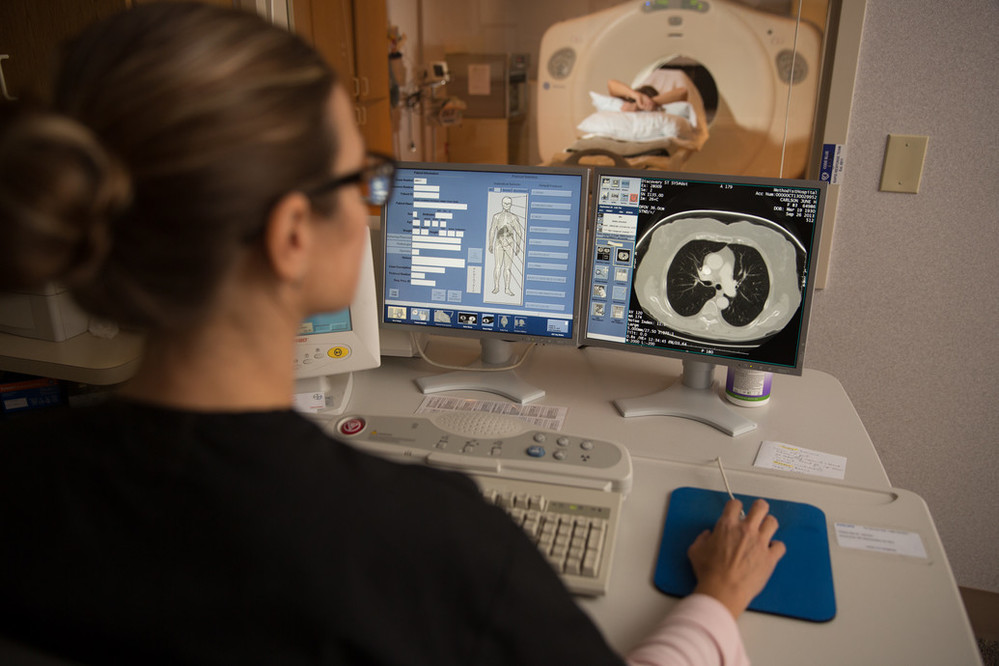
After reviewing her history, he had a simple suggestion: Get a low-dose computed tomography (CT) scan of her lungs.

A Powerful Tool
Lung cancer is the second most common cancer in men and women in the U.S. and the leading cause of cancer death. It’s estimated that over 235,000 cases of lung cancer will be diagnosed this year in the U.S. and over 131,000 people will die from the disease.
For many people with lung cancer, symptoms don’t appear until the disease is more advanced. By then, it can be more difficult to treat.
That’s where a low-dose CT scan comes in. The scan exposes the patient to less radiation than a standard chest CT scan but is far better than older imaging methods at detecting abnormalities in the lungs earlier and when they’re smaller. It’s also covered by most insurance plans and Medicare/Medicaid. Methodist Hospital Foundation also offers financial support to patients without insurance, Medicare or Medicaid coverage who may need assistance with co-pays or out-of-pocket expenses.
The procedure is a key part of the Methodist Lung Cancer Program, which takes a multidisciplinary approach to identifying and treating the disease.
“This is like going from a 1950s black and white television to HD,” said Methodist cardiothoracic surgeon John Batter, MD. “A CT scan gives you a much clearer picture.”
The result is more lung cancers caught earlier – before symptoms are present and outcomes are worse.
“It’s just amazing to me that that’s able to happen, and it’s underutilized,” said Methodist pulmonologist Chris Shehan, MD. “There is a small amount of radiation, but in my mind, it’s worth it. If we can catch these patients with an early lung cancer, diagnose them and treat them, their chance of five- and 10-year survival goes up dramatically.”
Joellen’s history is what caught Dr. Welstead’s attention. She checked all the boxes providers look for when referring patients for the low-dose CT scan. Patients are eligible for a screening if they:
- Are 50-80 years old
- Have a 20 pack-year smoking history (one pack per day for 20 years or two packs a day for 10 years, etc.)
- Are current smokers or have quit in the past 15 years
- Have no symptoms of lung cancer

As a radiologic technologist and mammographer, Joellen knows the importance of screening and early detection. She also knows that people have been putting off doctor’s appointments and screenings because of COVID-19. This was the first time she’d heard of a screening to detect lung cancer, but she didn’t hesitate.
“I thought, well, it can’t hurt,” she said. “I went in on a Friday. It took 10 minutes. They got back to me the next week.”
Faster Treatment, Better Outcomes
Within days, Joellen received troubling news: The scan had detected a suspicious small nodule. But she soon learned she was in good hands. She was immediately scheduled for the weekly lung cancer clinic at Methodist Hospital.
Instead of having patients book multiple appointments over potentially several days or weeks, the clinic creates “a one-stop shop for a patient,” Dr. Batter said.
The clinic aims to go on the attack faster by bringing together a team that includes specialists in pulmonology, radiology, pathology, oncology and thoracic surgery. In the morning, a patient will have a pulmonary function test, connect with a nurse navigator and be scheduled for a biopsy if necessary. The patient then heads home, but the multidisciplinary team’s work is just beginning. It reviews the dozen or so cases from that day and forms a consensus on how to proceed. That same afternoon, staff are able to schedule appointments with patients based on the team’s recommendations.
“All the disciplines that are involved in lung cancer care are together making recommendations for each patient’s specific situation,” said Deborah Meyers, BSN, OCN, program manager for the lung cancer clinic. “It’s very important. The faster you get treatment, the better the outcomes are. Having those groups together, you can get moving on the different testing, biopsies or whatever you need a little bit quicker.”
After Joellen met with Dr. Shehan, a biopsy revealed that while her 8-millimeter nodule was cancerous, it was in the earliest stage and very treatable.
“When I first heard, I did break down,” she said. “But then I talked to the doctors. They told me how small it is and that they recommend having the surgery – and if it hadn’t spread, I wouldn’t need anything else. The fact that all those doctors working together projected that outcome gave me the confidence.”
She was soon scheduled for surgery with Dr. Batter, who was able to maneuver between her ribs to remove the nodule as well as lymph glands near her sternum. After several days of recovery at Methodist Hospital, Joellen returned home with renewed peace of mind and a deep appreciation for the team that cared for her.
“Within a month’s time, they got all this done,” she said. “If I had not gone in for that test, by the time I started feeling sick or had symptoms, it could have been way too late.”

“It Can Save Your Life”
For the next two years, Joellen can expect to meet with Dr. Shehan and have a CT scan every six months. After that, the scans and meetings will be annual, but Dr. Shehan doesn’t expect her cancer to return.
And Joellen recently received more good news. Her husband, Dan, a former smoker, had a low-dose CT scan that came back clean in December. Their experiences have given her a new outlook.
“Right now, it’s to enjoy life,” she said. “I’m not going to be putting things off anymore.”
She and Dan have a travel bucket list that spans the globe, and they plan to spend more time with their five children and 11 grandchildren.
They’re powerful examples of the importance of screenings and early detection. Nationally, Meyers said, about 4% of eligible people get screened. Dr. Shehan would like to see low-dose CT scans as well-known and utilized as mammograms and colonoscopies.
Joellen agrees and is doing her part.
“I’m just telling anybody I know, talk to your doctor. See if you qualify to have this test, because it can save your life.”
More Resources
- Learn more about lung cancer screening at Methodist.
- Read more stories about cancer care at Methodist.
- Follow Methodist on Facebook, Twitter and Instagram.


