Cancer Care
'Everybody Needs Somebody Watching Their Back'
Published: May 17, 2022
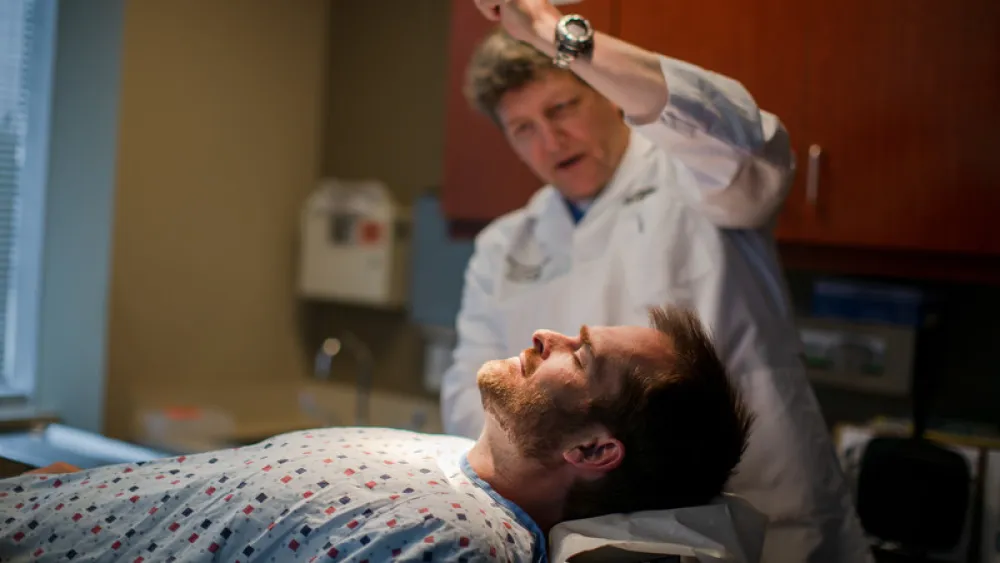
He has fond memories of playing sports outdoors and occasional boating trips. He even recalls a few sunburns, because when it came to sunscreen, “I remember having it and wearing it, but I don’t know how much it was really stressed.”
What the blue-eyed and lighter-haired structural engineer can’t remember is what exactly compelled him to start seeing dermatologist Scott DeBates, MD, at Methodist Physicians Clinic West Dodge Medical Plaza.
“It was probably the fact that I have moles all over my body,” Dusten said. “I just figured I should get them checked.”
His first full-body skin exam was in 2006. He returned the following year for another routine check. He nearly walked away scot-free.
“I almost told him he could stand up – that he was good to go,” Dr. DeBates said. “That’s when he pointed to his leg and asked me, ‘What do you think about this one?’ It was all one color, it had smooth, even borders, so I said, ‘It looks OK. How long have you had it?’ He said, ‘About a month.’”
Dr. DeBates, who specializes in Mohs micrographic surgery, wasted no time. He removed the mole for further evaluation.
An Unforgettable Diagnosis
While much of that appointment remains a blur for Dusten, he’ll never forget that follow-up phone call from Dr. DeBates.
“I was at my office. Midday. I was sitting at my desk,” Dusten said. “I answered the phone, and he said, ‘We found cancer.’ Everything just froze.”
Dusten had malignant melanoma, a deadly type of skin cancer that develops when melanocytes, the cells that give our skin color, turn cancerous and start to multiply.
He took a deep breath before calling his wife, who had given birth to their third child just two weeks prior. At 31 years old, Dusten wondered if his time was growing near.
“I wasn’t afraid of dying,” he said. “I was afraid of my kids growing up without a dad. I was afraid of my wife raising them without a husband.”
Dusten was immediately referred to James Reilly, MD, a surgical oncologist with Methodist. Dr. Reilly determined that Dusten’s cancer had spread to only one of his sentinel lymph nodes, which are the first in a chain of lymph nodes to collect metastasizing cancer. Finally, there was a glimmer of hope.
In May 2007, Dusten began a year of immunotherapy. From that point on, he and his family became increasingly vigilant.
“Not only about sunblock,” he said, “but the clothes we’re wearing, the hats we’re wearing, the time of day we’re out. Just anything we can do to minimize our sun exposure.”
“And I can’t stress that enough,” Dr. DeBates said. “It’s not just about sunscreen. Sunscreen makes people feel safe. They use it as an excuse to stay in the sun longer. If sunscreen was the fix-all, you’d think that with its invention, we’d have seen a reduction in skin cancer, but we haven’t. We’ve seen an explosion of skin cancer. If you have to be in the sun, yes, use it and reapply it. But I caution everyone against believing it’s a perfect shield.”
Men and Melanoma
More than 190,000 cases of melanoma will be diagnosed this year. While some may consider it a woman’s disease, the majority of people diagnosed with melanoma are white men over 55. And men ages 15 to 39 are more likely to die of melanoma than women of the same ages.
“If early detection is key to survival, that statistic tells me that men are not paying as close attention to their skin as women,” Dr. DeBates said.
While it’s never a bad idea to schedule a skin exam with a dermatologist, “don’t assume you’ve done your duty,” Dr. DeBates added. “You need to look. You’re the one who’s right there. Look at what you can and get a friend or family member to look at the spots you can’t see, like your back. Everybody needs somebody watching their back.”
While those with lighter hair, skin and eyes are most at risk for developing melanoma, he urges everyone to look for changes in the color, size and shape of existing moles.
He also stresses awareness of new and developing moles.

In Dusten’s case, the change was a mole that appeared out of nowhere, but he recognized it. And because of that, he’s alive.
“I believe I’m here for a reason. I don’t know what that reason is. We’ll find out,” the survivor and now father of five children said. “Maybe we already have.”
More Common than Melanoma
Basal cell carcinoma and squamous cell carcinoma are cancers that develop in the upper layers of the skin. Caused by years of accumulated ultraviolet radiation exposure, they tend to develop on areas of the body that receive the most sun, such as the face, hands and forearms.
Close to 3 million basal and squamous cell cases will be diagnosed this year, and most of the time, the recommended treatment is surgical. Unfortunately, surgical removal of tissue in such cosmetically sensitive areas can result in scarring and disfigurement.

Squamous cell carcinomas are not quite as common as basal cell cancers and can pose a greater danger for metastasis.
Like melanoma, early detection of these cancers is key. Dr. DeBates commonly tells his patients: “Early detection of basal and squamous cell carcinoma leads to a smaller scar. Early detection with melanoma leads to a longer life.”
Photos by: Chris Thompson
More Resources
- Learn more about Methodist's dermatology services
- Read more from the Summer 2019 issue of The Meaning of Care Magazine


