Heart Health
COVID-19 May Increase Your Risk of Stroke - Even if You're Young
Published: May 15, 2020

As coronavirus disease (COVID-19) continues to spread throughout the world, our understanding of its symptoms and how it affects major organ systems has evolved. There are still so many unanswered questions. But what we know for sure is that COVID-19 doesn’t affect just the respiratory system – and there are increasingly worrisome links between the coronavirus and stroke.
COVID-19 has stroke practitioners on alert. Not only has the number of potential stroke victims calling 911 dropped significantly, but there’s also a rise in cases of younger COVID-positive patients suffering strokes – and severe ones.
Strokes Are Still Happening, but 911 Calls Aren’t
Fewer people have been calling 911 when they have signs of stroke. One recent study found that the number of people being evaluated for strokes at U.S. hospitals has fallen by nearly 40% during the pandemic. That doesn’t mean people aren’t having strokes; it means they aren’t calling for the help they need.
Why the sudden drop? Some people might be fearful of contracting COVID-19 at the emergency department. Others might be brushing off stroke symptoms as “not a big deal” and don’t want to “waste” resources during a pandemic. Still, others might be isolated because of social distancing, having no contact with friends and loved ones who might recognize signs of stroke.
At Methodist, we want to be as clear as possible: We are here, and we are ready to care for you. If you are having signs of stroke, call 911. This is a case in which the emergency department is for you. We screen all patients for COVID-19, and we have separate units established to care for COVID-positive patients. Our nurses, neurologists and therapists – they’re all here for you to start your recovery immediately and get you back to your baseline as quickly as possible.
Younger COVID-Positive Patients and Stroke
Stroke practitioners are also on the lookout for an apparent link between COVID-19 and an increased risk of stroke in younger populations. Medical experts are still trying to understand why COVID-19 is causing a higher number of blood clots in patients. And doctors are increasingly alarmed by COVID-positive patients in their 30s, 40s or 50s suffering the deadliest type of stroke – large vessel occlusions (LVOs). The average age of someone suffering from an LVO is 74.
What we’re now seeing across the country is that some younger COVID-positive patients are developing a stroke within 14 days of COVID-19 symptoms starting. Or others go to the emergency department to get treated for stroke and then test positive for COVID-19. For some, they experience no other established COVID-19 symptoms.
Stroke education for everyone in their 30s, 40s and 50s is more important than ever as we try to understand the link between stroke and COVID-19. The biggest lesson to remember: BE FAST.
BE FAST
We have a saying in stroke readiness: Time is brain. That was true before COVID-19, and it’s true now. Every minute that passes following a stroke could mean the loss of precious brain cells and can mean the difference between a positive and negative outcome. That’s why, when it comes to detecting a stroke, we urge everyone to BE FAST – whether you’re having one sign or several.
Each letter in the acronym BE FAST stands for a warning sign of stroke.
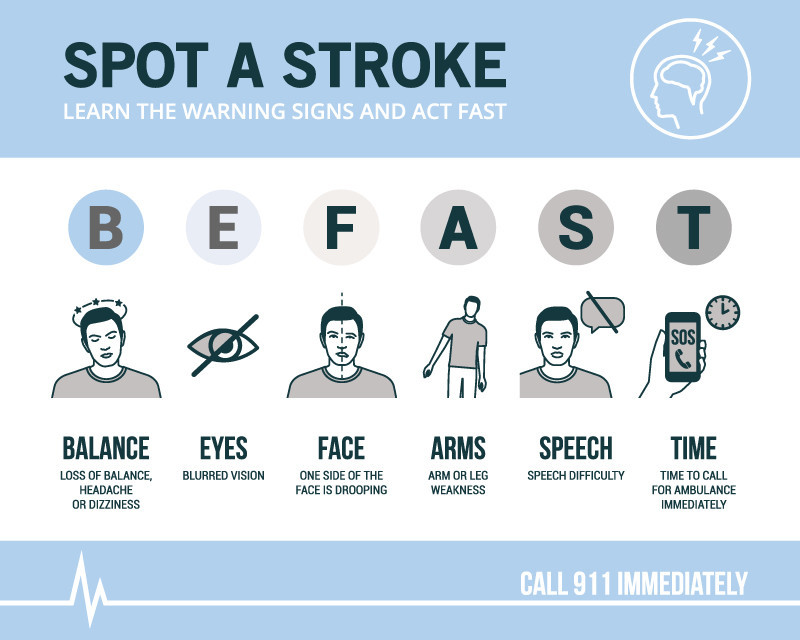
B – Strokes that begin in the posterior of the brain (which can account for up to 15% of all strokes) can often cause sudden changes in balance. You may experience dizziness or headaches as you try to maintain your balance.
E – Posterior strokes can also cause problems with your eyes. You may lose sight, experience doubled or blurred vision, or not see things to the right or left.
F – If you notice that one side of your face feels tingly and kind of droopy, that is a sign of stroke. It may feel like you just visited the dentist and had a shot of Novocain.
A – A loss of strength or weakness in your arm, leg or both, on one side of your body can be a key indicator of stroke. This asymmetry may feel like a tingling sensation or like you just can’t move one side.
S – If you are trying to talk but your words aren’t coming out normally, that speech difficulty is a sign of stroke. You may have difficulty understanding what a person having a stroke is saying. Words can come out slurred or garbled.
T – If you experience any of the symptoms above, time is of the essence. Call 911 right away.
Don’t Be Afraid to Call 911
Again, if you’re experiencing a sign or signs of stroke, call 911. Remember that time is brain. Do not drive yourself or have someone drive you. When you call 911, ambulance crews can inform our emergency department that a potential stroke patient is on the way. It allows us to save precious minutes when you arrive. The quicker a stroke patient can receive treatment, the better their chance of recovering from the event.
We understand you’re afraid during this uncertain time, but we’re here for you when you need us. What can you do now? Keep up those daily walks and any healthy habits you’ve formed while social distancing and staying at home. If you’ve lost your job and are worried about affording any stroke-preventing medications you’re taking, talk to your primary care provider about options and programs that can help. Keeping listening to your body, and educate yourself and your loved ones about stroke – no matter their age.
More Resources
- Learn more about stroke care at Methodist.
- Read what happens when the clock starts ticking on stroke.
- Learn more about the process of stroke recovery.
- Follow Methodist on Facebook, Instagram and Twitter for COVID-19 updates.


