
The Meaning of Care Magazine
‘He Cares With All of His Heart’: Volunteer Impacts Methodist Hospital Patients Through Simple Conversation
Published: Dec. 12, 2022

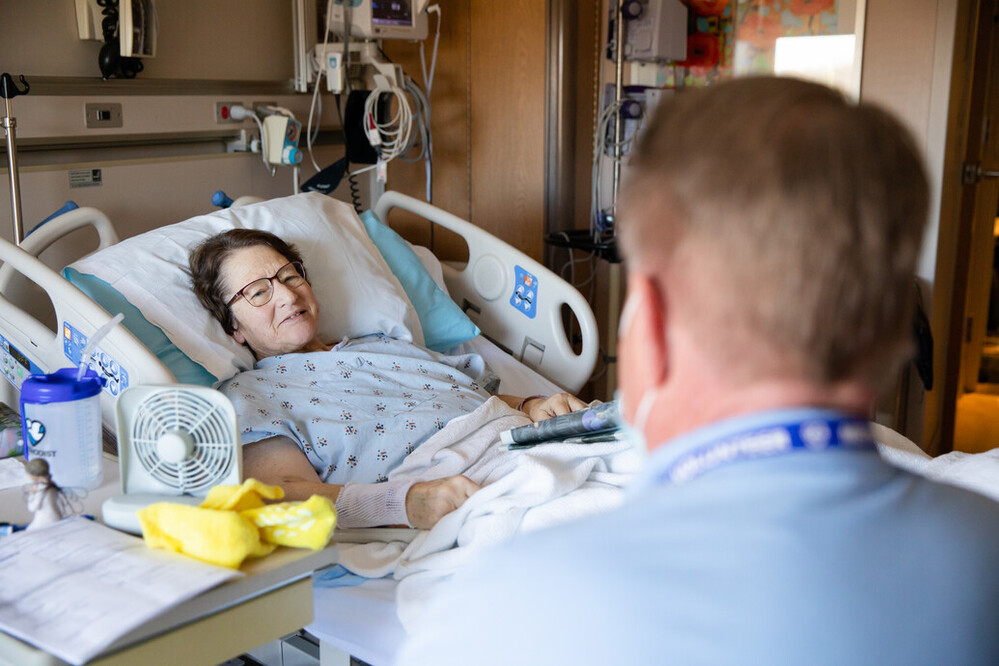
Volunteer George Zieg visits patient Dick Perrigan at Methodist Hospital in November.

It’s a moment that Teaira Homan, CNA, won’t forget.
A patient in Methodist Hospital’s Acute Care for Elders (ACE) Unit kept pressing her call button, requesting that staff to come to her room. The patient didn’t have immediate medical needs, but she was confused about her situation.
“It was nonstop, every two minutes,” said Homan, a restorative aide who helps patients improve mobility through individual and group exercises. “And then George came in.”
George Zieg, 72, a retired pediatric allergist and immunologist, volunteers by visiting ACE Unit patients three days each week.
“George went in there and probably spent 30 or 40 minutes with the patient,” Homan said. “He took his time. He talked to her. And I remember that after he left, I was worried because she hadn’t called.”
Homan went to check on the patient, and “my heart just shook,” she said.
“The patient said, ‘This young man came in and spent time with me. Even if he wasn’t my friend, he felt like my friend. He just talked to me.’”
“What did you talk about?” Homan asked.
“I don’t remember,” the patient replied. “It doesn’t matter. He made me feel special.”
Well-Rounded Care
Methodist’s Hospital’s ACE Unit is specifically tailored for patients 65 and older who have a variety of noncritical conditions. Some may spend a few days in the unit while others are there for weeks.
All ACE staff members have geriatric-specific education, and the unit aims to enhance mobility and independence while preventing or reducing functional and cognitive decline, delirium, falls, and other situations common for older patients.
Hospital Elder Life Program (HELP) volunteers like George offer additional support by spending time with patients over 70 to further combat delirium and encourage socialization, alertness and mobility, when appropriate.

“There are all kind of things that we need to do to help people heal,” said Ginger Gifford, MSN, RN, SCRN, service leader for the ACE Unit. “A lot of it has to do with science and medicine, but a lot of it doesn’t. I think having the HELP program and having someone like George involved with our patients promotes healing in a fuller way – which is what our nursing practice is all about.”
George saw firsthand during his working career how important the intangible aspects of care are. While he was initially fascinated with what he learned in medical school, he grew to value the personal side of medicine and the relationships he built with families. When he retired in 2014, that’s what he missed the most.
“I was privileged to think that they would share their most intimate facts of life with me, a stranger,” he said. “Over the years, I not only saw them or their kids, but their kids got big, and I saw their kids. That’s what I missed when I retired. I missed the patient interaction.”
In 2018, he learned about Methodist Hospital’s volunteer opportunities and decided he could positively impact patients through the HELP program. What he didn’t know is that his own health issues would soon threaten to derail his efforts.
Renewed Perspective
Around the time George began volunteering, he began losing his balance and falling while mowing his yard or performing simple tasks in the kitchen. As his symptoms intensified, he found himself falling more and experiencing temporary paralysis in his legs.
A neurologist diagnosed George with ataxia, a degenerative disease of the nervous system, but couldn’t identify a cause. Medication did little to help George, and by the summer of 2020, his condition was worsening. He soon traded the cane he once used to steady himself for a walker. He had trouble feeding himself with tableware, and he began choking on his food. His neurologist advised him to arrange skilled care.
George decided to seek a second opinion. A second neurologist set up an appointment at the Mayo Clinic in late 2020. Not long after, George took a turn for the worst. After a particularly bad fall, he was hospitalized and became delirious. He spent a week in the Methodist Hospital Critical Care Unit on dialysis, then another seven at the hospital as he gained enough strength to be transferred to an acute rehabilitation facility.
That’s when George finally began to turn the corner. His delirium had subsided, and his memory returned. He was working toward the goal of entering assisted living in a wheelchair when his second neurologist called with life-changing news. After studying the case further, the neurologist believed George had a deficiency of the antibody immunoglobulin E – likely causing the ataxia. He wanted George to begin taking vitamin E supplements.
The difference was almost immediate. Within a week, George began using a walker again. A week later, he was walking without assistance.
“I walked out the door two weeks after that,” he said. “It cured my ataxia.”
He resumed his volunteer duties soon after. Although he has other health challenges, they don’t keep him from visiting patients – now with renewed perspective about their journeys and his own.
“I think I appreciate my health more than I ever did,” he said. “And I just appreciate that I wake up every day and basically do what I want. That’s a lot more than a lot of people can do.”

Nothing Off-Limits
George’s dedication to his volunteer shifts is well known to hospital staff.
“He’s here Monday, Wednesday and Friday without fail,” Gifford said.
But once he’s with a patient for what he calls “talk therapy,” he lets them steer the conversation.
“He has no agenda,” Gifford said. “He doesn’t set it up as if he’s got a limited amount of time. He’s comfortable with silence, too. He can tell when it’s time to let someone sit for a minute. He’s just calmly present.”
George’s visits can range from few minutes to an hour, and topics often include a patient’s family, pets, career or memories from decades past.
“I’m not too far off from some of these patients,” he said. “So it brings relevance to their history when I talked to them because I recall what things were like years ago. I enjoy that, too, because it brings up good memories for me.”
Oftentimes in just a few minutes, George said, he’s established an atmosphere of trust where nothing is off-limits.
“They’re sometimes telling me very intimate thoughts, especially life or death, going into hospice. And I know that’s difficult for them to talk about. There are people who break down and cry sometimes. They need to vent at times. Even if it’s to a stranger, they feel like they’re being heard.”
“He’s the Real Thing”
On a recent Monday morning, George was back in the ACE Unit making his rounds. His first stop was to visit Karen Bedlan, who arrived at the hospital two weeks earlier with back pain that doctors identified as liver cancer. She’d need surgery and chemotherapy. But as she waited for details on those next steps, she was glad to pass the time with a visitor.
George had visited Karen before, and they quickly fell into comfortable conversation about her diagnosis, family and dog.
“He’s easy to visit with, and I’ve enjoyed our conversations,” Karen said. “He’s made me feel good, and he’s very attentive when I talked about something.”
Next up for George was a stop down the hall to see Dick Perrigan. Dick had tripped and injured his knee and shoulder a few days earlier, but prescribed steroids caused his blood sugar to spike to levels requiring hospitalization.
Now, with his condition stabilized, Dick was equally pleased to have a friendly face to talk to. He came away equally impressed with George’s compassion for patients and devotion to volunteer work.
“He’s the real thing,” Dick said. “You can’t fake that. He’s got a persistence – a drive to do some good for others."
They’re traits that are on display each time George walks the halls of the ACE Unit. With each volunteer shift he works, patients discover what staff members have long known.
“He’s an amazing person,” Homan said. “He cares with all of his heart.”
More Resources
- Read more from the winter 2022 issue of The Meaning of Care Magazine.
- Find volunteer opportunities at Methodist Hospital and across Methodist Health System.
- Learn more about Geriatric and Senior Services at Methodist.


