Today's Medicine
It’s Time To Return to Cancer Screening
Published: July 7, 2021

Did you delay your mammogram during the COVID-19 pandemic? What about your colonoscopy? Have you scheduled that low-dose lung CT scan, or are you still dragging your feet?
As we continue in this new phase of the COVID-19 pandemic and vaccination rates rise, it’s imperative that we shift our mindsets from crisis management back to preventative care. That’s why Methodist Health System is partnering with the American Cancer Society and the American College of Surgeons Commission on Cancer as we join health systems and organizations across the country to improve cancer screening rates and stop cancers as early as possible.
The message is clear: It’s time to return to cancer screening.
Danger in Delaying
We know that the number of people newly diagnosed with cancer in the U.S. and around the world decreased significantly during the pandemic. We also know that cancer screenings dropped and even came to a halt for several weeks. The conclusion? An untold number of cancers have gone undiagnosed and untreated. The National Cancer Institute predicts that in the next 10 years, the U.S. will see 10,000 excess deaths from breast cancer and colorectal cancer alone because of the COVID-19 pandemic.
When it comes to cancer, a one-year delay can be a long time. For people who continue to put off screenings that were due earlier in the pandemic, that delay is getting closer to two years. At Methodist, we worked hard to ensure that everyone’s appointments were rescheduled after we paused screenings out of an abundance of caution. Today, we’re no longer seeing a drop in appointments. But we know there are community members out there who are due or overdue for regular screenings.
Screening Recommendations

If you believe you’re due for a routine cancer screening, call your provider today. Unsure? Get a refresher on when you’re due for what screenings.
Breast
- Beginning at age 40, women should have an annual mammogram.
Cervical
- People with a cervix, age 25 to 65, should have a primary human papillomavirus (HPV) test every five years.
- Alternately, they can be co-tested every five years with an HPV test and Pap test, or be tested every three years with a Pap test alone.
- People older than age 65 with a cervix can stop being screened as long as they have 10 years of regular screening with normal results.
Colorectal
- People at average risk of colorectal cancer should start regular screening at age 45. Testing frequency depends on the type of test used.
- For people age 76 through 85, screening should be based on personal preference and life expectancy.
- People over 85 should not be screened.
Lung
- People age 50 to 80 should receive annual low-dose lung CT scans if they also:
- Have a 20 pack-year smoking history
- Are current smokers or have quit in the past 15 years
- Have no symptoms of lung cancer
This is not a comprehensive screening list. There are other cancers to get screened for, including prostate, skin and head and neck. A great place to start is by making an appointment with your primary care provider.
Screening Works
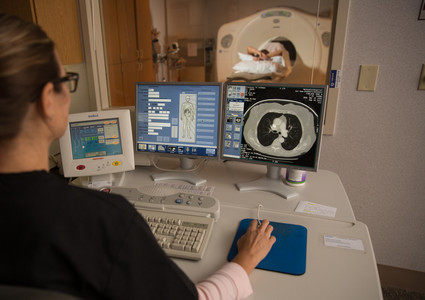
As a pulmonologist, I see firsthand that cancer screening works. Thanks to changes in the low-dose lung CT scan requirements, we’re catching more lung cancers in earlier stages.
It’s simple: The earlier we catch cancer, the better the outcome. And for annual screenings like mammograms and low-dose lung CT scans, radiologists can look at scans from year to year and detect the smallest changes before they become something more serious.
So, I join everyone at Methodist in encouraging you to return to cancer screening. Our clinics and hospitals are safe. And we’ve reached a point in the pandemic where the benefit of cancer screening outweighs any risk of COVID-19 exposure. We look forward to seeing you again for screenings and fighting by your side to stop cancer as early as possible.
For more information on screenings or to find a provider, visit bestcare.org.
More Resources
- Learn how a low-dose lung CT scan saved one former smoker's life.
- Learn more about mammography at Methodist.
- Learn more about lung cancer screening at Methodist.


