Today's Medicine
Methodist Hospitalists Offer Expert Care Around the Clock
Published: March 16, 2020


Randy Lang had just gotten off of work, and he was having trouble breathing.
“It was like my stomach was in my throat, cutting off my airway,” said Randy, who has heart failure.
Making the long drive from work in La Vista to his home in Red Oak wasn’t an option. Instead, he headed for the Methodist Hospital Emergency Department. Soon after being admitted to the hospital, he met Jocelyn Bailey, MD, and knew he was in good hands.
“That first impression says it all,” he said. “She cares about people.”
As a hospitalist, Dr. Bailey is dedicated to managing the care of patients like Randy. Her role involves working with hospital nurses, specialists and other staff to assess patients’ needs and coordinate specialized care – all while updating primary care providers (PCPs). The goal isn’t to replace PCPs, but to collaborate with them.
“Everyone brings a different dynamic and a different piece of information that can be helpful to a patient,” Dr. Bailey said. “I think that’s a really beautiful part of health care. No one person can do it all, but we all can work together to help someone.”
It’s a modern approach to medicine that plays out daily at Methodist Hospital, Methodist Jennie Edmundson Hospital and Methodist Fremont Health.
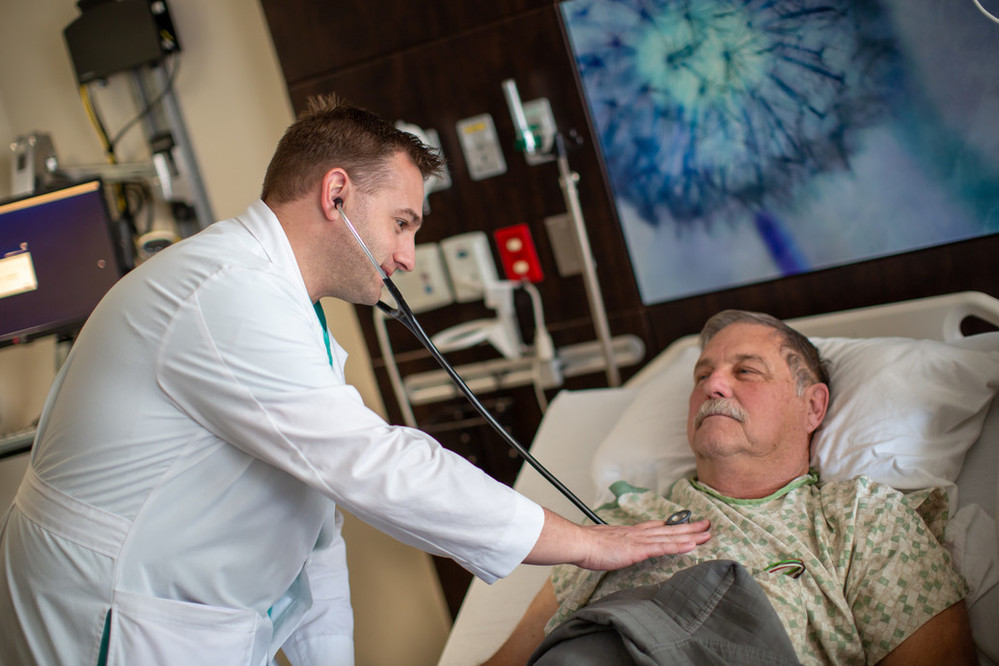

Providing Peace of Mind
While it was once routine for PCPs to visit their patients in the hospital, Methodist is seeing success with its hospitalist program. With more than 50 hospitalists and 24/7 staffing, patients receive expert care almost instantly.
“We can look at test results within an hour of them being available and move forward,” said Evelyn Reher, MD, a hospitalist at Methodist Jennie Edmundson. “If a patient does have an acute problem, we can be at the bedside within minutes.”
That speed can translate to a shorter and more efficient hospital stay – something Marvin Bales experienced firsthand.
Two days before Christmas, Marvin began experiencing excruciating chest pain.
“From one to 10, it was 11,” he said.
He ended up at the Methodist Fremont Health Emergency Department, where a CT scan revealed a blood clot in his lung. Hospitalist Jeffrey Arnzen, MD, managed his care.
“The doctor said, ‘That could have killed you,’” Marvin said.
But thanks to a combination of pain medication and blood thinners, his condition had improved by that afternoon, and he was eager to return home.
“I’ve got a lot of things I can get done tomorrow,” he said, describing various projects and the Christmas gift he had yet to pick up for his wife.
Cases like Marvin’s are exactly why Dr. Arnzen became a hospitalist.
“I like taking care of the acutely ill,” he said. “When people have a sudden illness, I can usually help them recover pretty quickly. But I can also spend as much time as I need with any particular patient or family to explain exactly what’s going on.”
Dr. Arnzen stopped by one last time to visit Marvin on the morning of Christmas Eve. He would have to continue taking blood thinners, but by 6:30 a.m. – less than 30 hours after his chest pain began – he was free to tackle his to-do list. He had Dr. Arnzen and the Methodist Fremont Health staff to thank.
“He’s a good guy,” Marvin said. “He explained it all really well.”

Communication and Trust
Methodist’s hospitalist model is built on communication and collaboration. From admission to discharge, hospitalists and PCPs are partners in a patient’s recovery.
For example, if internist Melissa Hernandez, MD, is seeing a patient at Methodist Physicians Clinic Regency who needs to be hospitalized, a hospitalist is only a phone call away. In a matter of minutes, she can secure a room and supply information about the patient’s condition and medical history. The time that’s saved benefits patients and hospital staff.
“That’s nice to have that warm handoff,” Dr. Hernandez said. “Having them available frees me up to really focus on taking good care of patients in the clinic.”
The communication continues through a patient’s hospital stay. Providers like Dr. Hernandez are kept up-to-date on a patient’s status with regular updates via the electronic medical record, messaging and phone calls. Meanwhile, they’re quick to send a message or pick up the phone to relay important or nuanced information that may not appear on a patient’s record. And at the end of a hospital stay, a hospitalist’s detailed discharge summary lays the groundwork for a patient’s care as they return to see their PCP.
“There’s really nice communication both ways,” Dr. Hernandez said. “I trust our hospitalists a lot. I would trust them taking care of my family members.”

Finding Success One Patient at a Time
Methodist has made it a priority to develop relationships with hospitals and providers in smaller communities. As its hospitals and clinics build on their regional reputation for providing outstanding specialized care, the hospitalist program will only grow. Outcomes like Randy’s and Marvin’s make it easy to see why.
After several days at Methodist Hospital, Randy said his breathing and other symptoms of heart failure had improved. So had his spirit. He told stories and joked around as Dr. Bailey checked in and listened to his lungs.
“That’s how we know people are actually starting to feel better a lot of the time,” she said. “Their humor and sarcasm come back.”
Jokes aside, Randy was grateful for Dr. Bailey and his care at Methodist.
“When people get sick, this is the place to be,” he said. “I’m thankful for everybody’s teamwork here. I wouldn’t be here today if it hadn’t been for you guys.”
Photos by Daniel Johnson and Chris Thompson.
More Resources
- Learn more about Methodist's hospitalist program
- Read more from the spring 2020 issue of The Meaning of Care Magazine


