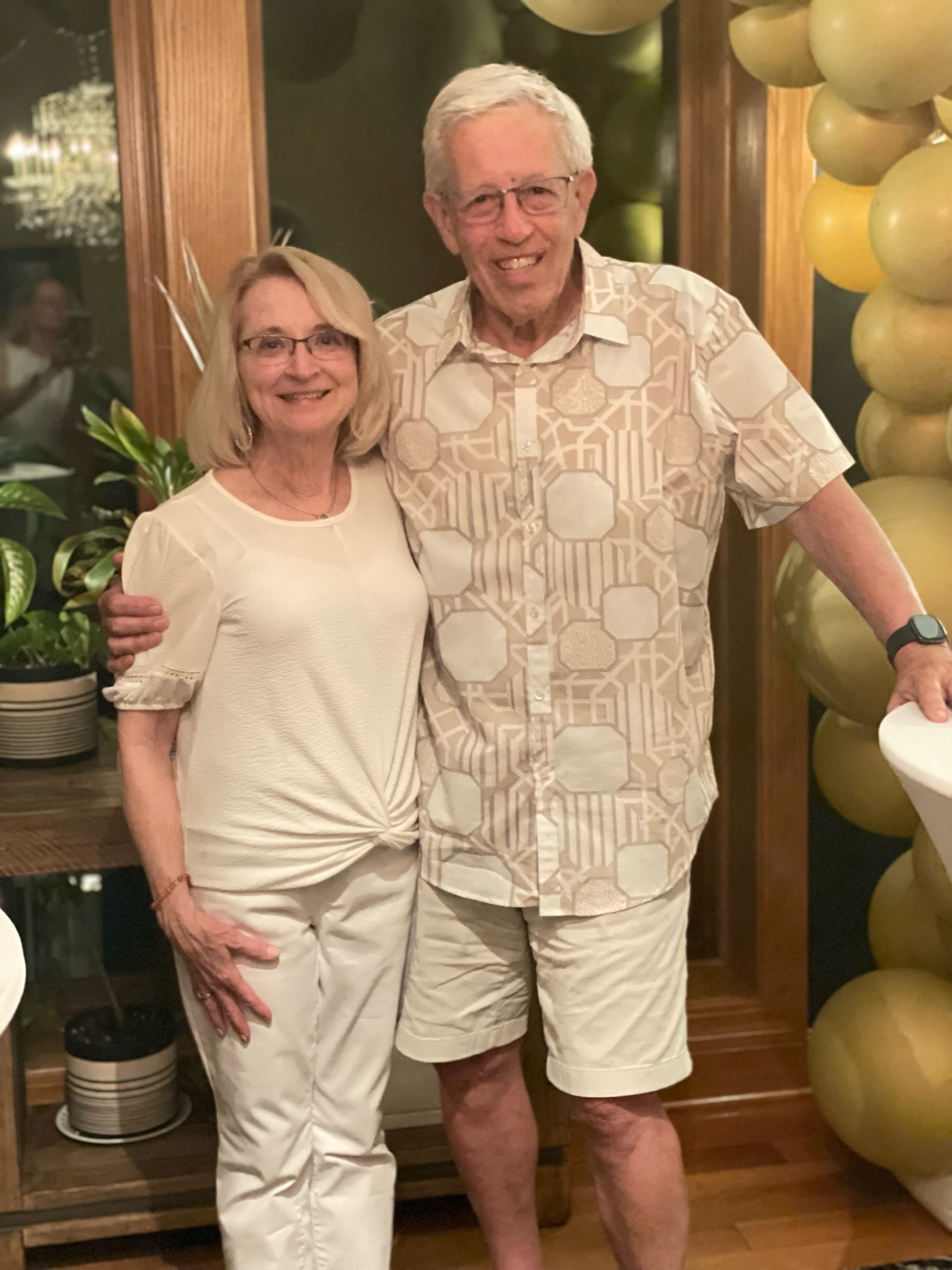
Cancer Care
Pancreatic Cancer Survivor Receives Treatment Close to Home at Methodist’s Nationally Recognized Cancer Center
Published: Nov. 30, 2022

“It’s been a rough journey, but it’s been a good journey, too,” said John Naatz, who was diagnosed with pancreatic cancer in the spring of 2021.
Because his cancer was caught early, John, 73, was able to have his tumor surgically removed, and he didn’t have to leave Omaha for the procedure. He chose to follow a treatment plan from Methodist Estabrook Cancer Center (MECC), which is recognized as the region’s only National Pancreas Foundation (NPF) Cancer Center.
“Having an accreditation like that and what is says about our center is definitely something that gives our patients comfort and confidence with having their treatment done here,” said surgical oncologist George Dittrick, MD, program director for pancreatic cancer treatment at Methodist.
Staying Home
In April 2021, John’s blood work at a routine cardiology appointment revealed concerning liver enzyme levels. So he made an appointment with his Methodist primary care provider, James Steier, MD, who scheduled an endoscopic biopsy.
On May 11, 2021, the biopsy revealed a cancerous tumor blocking John’s bile duct at the head of his pancreas.
“I was having absolutely no symptoms, so this came as a complete shock to me,” said John, who was referred to Dr. Dittrick and medical oncologist Timothy Huyck, MD, with Nebraska Cancer Specialists.
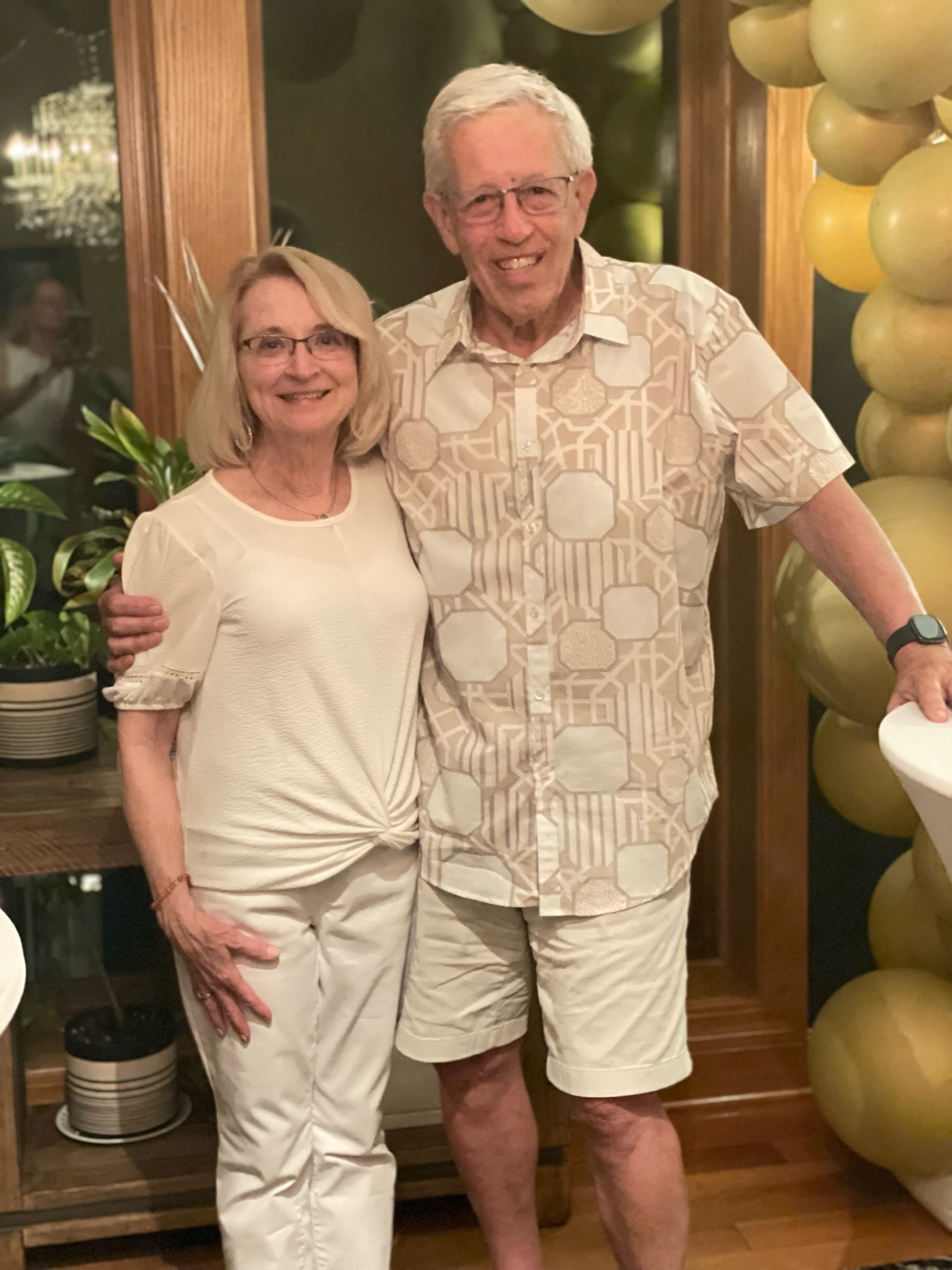
John decided to do some shopping around within the region. Some family and friends also urged him to look into Mayo Clinic, MD Anderson Cancer Center and The Johns Hopkins Hospital. But after meeting with Drs. Dittrick and Huyck, John ultimately decided to stay home.
“I told my wife, ‘I think I’m going to get tremendous care right here in Omaha.’”
He did.
But he also received much-needed support from family and friends.
“If you can receive cancer care from the comfort of your own home, sleep in your own bed, be around friends and family you need as part of your support system, and still get first-class treatment – that’s the best it gets,” Dr. Dittrick said.
Catching the Cancer Early
According to Dr. Dittrick, one of the problems with pancreatic cancer is that there isn’t a good tool for early diagnosis or screening.
“Some of the biggest advancements in other common cancers isn’t because of surgery being better, but because of picking up those cancers a lot earlier with screening methods like mammograms and colonoscopies,” Dr. Dittrick said. “Pancreatic cancer doesn’t have an equivalent screening modality.”
In John’s case, since he wasn’t experiencing abdominal pain or digestive issues – symptoms often linked to pancreatic cancer – the concerning blood work was the only sign that something was off.
It’s estimated that only 20% of pancreatic cancer patients are eligible for surgery. In most cases, the cancer diagnosis comes after the cancer has spread to other parts of the body and is more advanced.
“For any chance of cure, the tumor has to come out at some time,” Dr. Dittrick said. “Chemo and radiation play a big part in treatment, but you have to be able to remove it. And if four out of every five patients with a new diagnosis don’t have that option, then you’re stacked with some pretty bad odds from the get-go.”
John received six rounds of chemo before Dr. Dittrick performed the Whipple procedure on Sept. 28, 2021.
Despite some post-operative pain, John was grateful to have spent only five days in the hospital. And although later pathology showed that the cancer had spread to lymph nodes near the primary tumor, six more rounds of chemo and 28 radiation treatments have yielded clear scans since.
“I’m getting stronger every week,” John said. “My energy level is improving and I’m able to get back to a quality of life that I experienced prior to the diagnosis.”
Taking the Time To Explain the Plan
One of the things John appreciated most about Dr. Dittrick was the time he took, the drawings he sketched and the charts he used to fully explain the diagnosis and treatment plan.
“It was just wonderful,” John said. “It gave both my wife and me this tremendous peace of mind.”
“There’s a lot of uncertainty and a lot of unknowns,” Dr. Dittrick said. “You can’t take a patient through medical school and surgical residency, unfortunately, but you can give them a pretty good understanding of their specific diagnosis.”
And now, John has a solid understanding of what survivorship entails.
“Everyone that I worked with were tremendous professionals, very caring and empathetic,” he said. “Just wonderful people all the way around.”
“We have a good team,” Dr. Dittrick said. “And the more people that know about that, the better care we’re going to be able to provide to some of those people who deserve to have that quality of care.”


