
The Meaning of Care Magazine
Physical Medicine and Rehabilitation Team Offers Treatments To Minimize Pain, Help Patients Get 'Back to Life'
Published: April 10, 2023For the past 20 years, Richard Peterson, 91, has volunteered with the American Baptist Churches of Nebraska. He spends about eight hours each week in the offices talking on the phone or visiting with other staff members. On the weekends, he attends worship services at Baptist churches in the area and meets with pastors to address their needs.
But this past summer, Richard had to scale back his volunteer hours because he was experiencing back pain.
He also had to limit time with grandchildren and great-grandchildren who live near his northwest Omaha home.

After an appointment with his Methodist Physicians Clinic primary care physician, Mark Mahloch, MD, and a meeting with a neurosurgeon, Richard was directed to Jeremy Gallant, MD, a physiatrist with Methodist’s Physical Medicine and Rehabilitation (PMR) group.
In early December, Dr. Gallant provided Richard relief with a radiofrequency ablation – a minimally invasive outpatient procedure that involves sending radiofrequency waves into a needle electrode to create heat and destroy specific nerves that are causing pain.
“They hope the outcome will be no pain for at least a year and maybe two,” said Richard, who quickly returned to his regular volunteer work and spent the holiday season pain-free. “So that was good news.”
Providing Pain Relief
Dr. Gallant is one of seven PMR providers at Methodist who are trained to treat conditions that cause pain or limit function.
He joined the team in 2014 and introduced radiofrequency ablation as a way to offer relief to patients who suffer from life-limiting back or neck pain. Before Dr. Gallant brought this technique to Methodist it was only being done at select locations in the area.
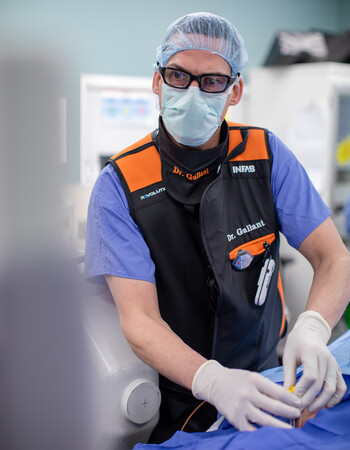
To ensure a patient is a good candidate for an ablation, trial injections are performed to determine whether specific joints in the spine are causing the pain. If the injections provide temporary relief, an ablation is scheduled.
The ablation destroys individual nerves near the problematic joints and ideally provides relief for up to 18 months. There’s a 50% chance that the nerve will regenerate and cause similar pain, but the procedure can be repeated.
Dr. Gallant performs nearly 250 ablations each year.
“Game Changer”
The patients Dr. Gallant treats include retired individuals, like Richard, who are hoping to enjoy leisure activities. He also helps younger patients who desire better, less painful work and home lives.
Jackie Hoff, 40, has experienced chronic headaches since sixth grade.
She’s met with physical therapists, chiropractors, doctors and specialists, but she’s never received sufficient relief.

Jackie also took pain medication daily, which left her with drowsiness at work and minimal energy at home.
As a surgical technician at Methodist HealthWest, she heard about Dr. Gallant’s radiofrequency ablation procedure. Although intrigued, she was skeptical.
“I have done so many different types of things, so I thought, here we go, we’re going to try something, and it’s not going to work again.”
Jackie received her first ablation treatment in 2020. It took a few weeks for the full effects to kick in, but she noticed quite a difference.
She woke up feeling refreshed, had energy at work and could enjoy time with her two children at home.
“It’s definitely been a game changer,” she said.

Kelly Williams, BSN, RN, a Methodist HealthWest surgery core coordinator, received an ablation in February 2021.
She initially thought her pain was heartburn, but Dr. Gallant informed her that a radiofrequency ablation might help because the pain was actually coming from her back.
Kelly believes the relief she received from the ablation allows her to take better care of patients and spend more time with her kids at home.
“It’s all about that quality of life that everybody is looking for,” she said. “Sitting in pain every day is just not a way to live.”
Stimulation Offers Hope
In addition to radiofrequency ablations, the PMR group has other cutting-edge procedures. Physician Jery Inbarasu, MD – who joined the team in the summer 2022 – added spinal cord stimulation to Methodist’s in-house offerings.
Patients eligible for spinal cord stimulation have already exhausted conservative methods of managing nerve-related pain, such as physical therapy, medication and even surgery.
“Some of these patients have probably lost hope that they’re ever going to have effective treatments,” Dr. Inbarasu said. “And I think this gets them back to a level of functionality that they want to have.”
Spinal cord stimulation involves two procedures. The first is a trial, sending wires through a needle into the back and then securing those wires to the skin and connecting them to an external stimulation device. The device sends a small amount of electricity, which can be controlled by a wireless remote control, directly onto the spinal cord to interrupt pain signals from reaching the brain.
If the trial is effective – meaning the stimulation positively changes a patient’s quality of life – a permanent procedure is scheduled.
That procedure is similar to the first. But this time, the wires are secured under the skin and connected to an implanted device – similar to a pacemaker.
When spinal cord stimulation was developed more than 50 years ago, the goal was to decrease a patient’s pain by 50%. But thanks to advancements in technology, many patients are now experiencing closer to 70% relief. And since Dr. Inbarasu joined Methodist’s PMR team, more patients are being presented this option.
“It’s been really rewarding to treat some of these patients because they usually see a pretty big change, and it changes the trajectory on where they’re going with their lives,” Dr. Inbarasu said.
Working Toward Patient Goals
The PMR team, which includes Dr. Gallant, Dr. Inbarasu, Zachary Gustin, MD, Thomas Franco, MD and James Cult, MD, work closely with primary care physicians and physical therapists to ensure a collaborative approach for each patient’s individualized goals.
Michelle Ninemire, DPT, a physical therapist with Methodist Fremont Health, says it’s nice knowing that she can easily refer patients to the PMR group if she thinks they could benefit from something more than she can provide. She also works with patients who first received a treatment from the PMR group before meeting her.

“We’re both looking at the patient as a whole and wanting to restore their function and get them back to their quality of life,” Ninemire said.
Dr. Gallant receives many patient referrals from primary care physicians and physical therapists across the region.
The PMR providers also work closely with neurosurgeons and orthopedic surgeons through Methodist’s partnership with MD West ONE.
“Being able to reach out and discuss things with a primary care physician, catch one of the physical therapists that’s working with a patient and/or talking with the neurosurgeons is probably some of the most important work that I do,” Dr. Gallant said.
He enjoys being able to help patients receive the help they need and get them “back to life.”
“We don’t really save lives, but we make lives worth living.”
More Resources
- Read more from the spring 2023 issue of The Meaning of Care Magazine.
- Learn more about physical medicine and rehabilitation at Methodist.


