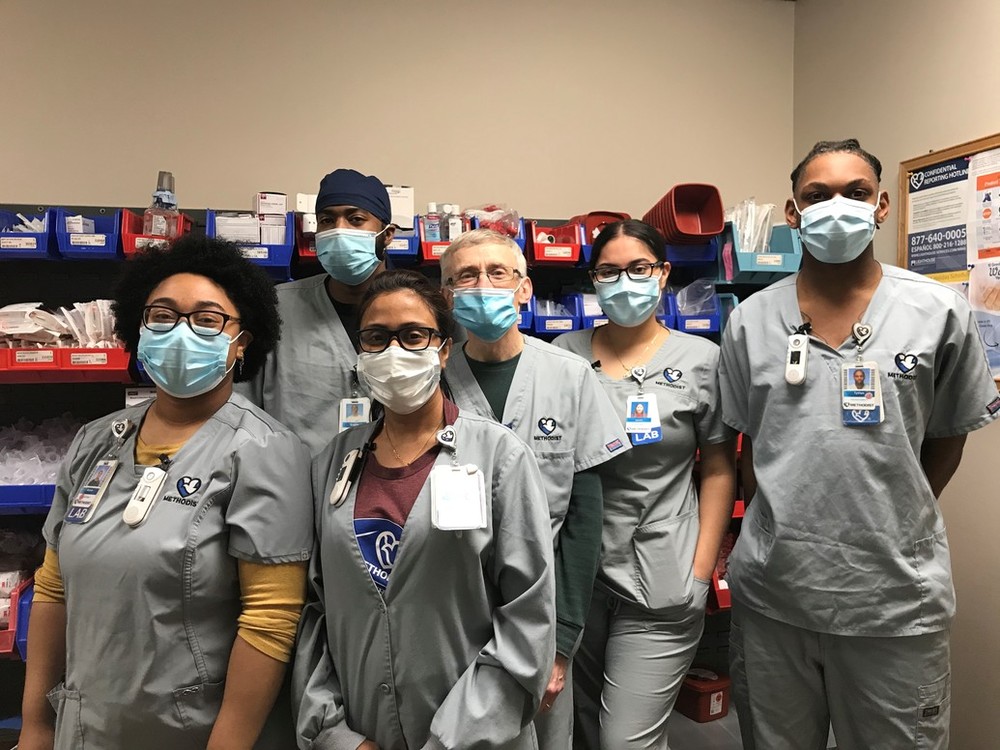
Unsung Heroes of COVID-19: Methodist’s Laboratory Staff Members Fill Crucial Roles
Published: March 25, 2021

The Methodist Hospital pathology laboratory team operates with a simple philosophy: There’s a patient behind every sample.
With nearly 200 staff members, the team fills a critical role in patient care by collecting and analyzing a variety of samples – which helps direct the care plans doctors and staff create. And while many staff members may never see a patient face-to-face, their work is guided by that mantra.
“We treat every sample like it could be from a family member or close friend,” said LaNett Whisler, MLS(ASCP), the service leader for microbiology and serology at Methodist Hospital. “We see it as just as important as if a patient were sitting there next to us. I love being able to do our part to treat patients who come through Methodist Health System.”
As the COVID-19 pandemic unfolded over the past year, the team has faced a series of challenges. But its members are among Methodist’s unsung heroes of the pandemic, rising to the occasion to make a difference and save lives.

Compassion Is a Must
Nearly every hospitalized patient requires some kind of laboratory test – of blood, urine, tissue or other specimens – to guide their treatment plan. The person often collecting that sample, a phlebotomist, might be the only member of the lab staff that a patient will ever see.
“Phlebotomists have to be compassionate people,” said Cyndi Schaer, PBT(ASCP) cm, the phlebotomy team leader for Methodist Hospital and Methodist Women’s Hospital. “We’re sticking people with needles. You can’t say it’s not going to hurt.”
That compassion has been needed more than ever during the pandemic – with some patients in isolation and others dealing with strict, but necessary, visitor policies.
“Human contact is so important for people’s mental and physical well-being,” Schaer said. “And when you take visitors out of the equation, then the patients kind of rely on the caretakers. They count on us to make their day a little better. Our team goes in and tries to make a bright spot in their day.”
Schaer also praised her tight-knit staff for its team mentality and flexibility. Early in the pandemic, hours were reduced when elective procedures were postponed and the overall number of hospital patients fell. Staff members picked up shifts on the health system labor pool to pitch in where they could. As elective procedures returned, the team had to rally to provide coverage for those patients as well as those with more pressing medical issues.
Then there were the evolving challenges with supply shortages and wearing personal protective equipment (PPE).
“At first, we would go room to room, and we would have to don and doff, put on and take off, the complete PPE,” Schaer said. “You had gloves, a gown, an N95 mask, eye goggles, another mask over the top of your N95. You had to be cleaning everything consistently.”
It was time-consuming and stressful, “but we knew that the hospital gave us everything that we needed,” she said. “It was never anything that we couldn’t overcome. We just had to make sure that we were paying attention to any new details that were being brought forth.”
As more was learned about COVID-19, PPE guidelines evolved to keep patients and staff members safe while easing donning and doffing requirements. Staff members also adjusted to their new normal, which now included new highs and lows. There were difficult times when patients struggling with COVID-19 were there one day and gone the next. And there were rewarding moments when a patient was moved out of isolation, moved out of the intensive care unit or discharged to go home.
“Those things are huge,” Schaer said. “That’s why we do this.”
Through it all, the phlebotomists focused on how important the entire lab team is to those successful outcomes.
“Good specimens give accurate results,” Schaer said. “We are the face of the lab, with an entire team of people in the lab who receive and process the specimens to give the best results.”

Behind-the-Scenes Experts
Hiding in plain sight on the Methodist Hospital campus is the Methodist Pathology Center-Schenken Pavilion. The 42,000-square-foot laboratory performs over a million tests a year for medical providers and facilities in Nebraska, Iowa and Missouri.
“Making sure those tests are done properly and the results are correct is paramount to making sure that the provider then provides the best care,” said Deborah Perry, MD, pathology medical director for Methodist Hospital. “If we don’t put out accurate results, the patient may not be treated appropriately.”

Even with so much capacity and expertise in house, there were plenty of challenges as the lab shifted gears to begin COVID-19 testing. Whisler remembers when Nebraska’s first COVID-19 patient was diagnosed in early March 2020.
“It kind of just exploded from there,” she said. “It was kind of a whirlwind. I went to work on Monday, and it was just meeting after meeting. ‘How can we bring in in-house testing?’”
Methodist and labs across the country faced the same complicated challenge, which included identifying which instruments they could perform COVID-19 testing on, acquiring testing supplies, making sure the test actually worked and adding it to their computer system – all before rolling it out to providers and patients.
Within about a month, the lab had limited testing up and running. Methodist was still sending many tests to national labs, but this was the first step toward a big goal: “We knew that we wanted to provide for the needs of everybody that came into our health system and not turn anybody away,” Whisler said.
As the lab’s capacity grew, Whisler was often working the phones, lobbying for the lab to get more testing supplies. One Saturday, she drove to Lincoln to pick up supplies on loan from Bryan Health – perhaps enough to last the weekend. It was the least she could do, she said, as she witnessed her medical lab scientists stretching to take on the added load.
As the “roller-coaster year” continued for Whisler and her staff, the lab continued adding testing capacity. By early December, as national suppliers caught up, the lab was able to handle tests from across Methodist Health System – sometimes as many as 200 a day.
Even as COVID-19 cases surged in the fall, the dedicated staff and processes they developed allowed the lab to handle the demand and serve more patients.
“There are incredibly smart techs in the lab,” Whisler said. “This is really their way to help without having that face-to-face patient care. We care just as much as a physician does for a patient, but we just express it in a different way. I particularly feel proud that we have helped our health system and our patients through this whole thing.”

Everyone Plays a Part
A year ago, getting COVID-19 tests results could take a week if sent to an outside lab. Today the Methodist Hospital laboratory team routinely completes COVID-19 rapid tests in 30 minutes and traditional tests in two hours. Each hospital in the Methodist system also now has the ability to perform COVID-19 testing.
That speed and testing accuracy is a testament to the work of all members of the laboratory team – from specimen collection to test result. And they’re proud to play their part in providing The Meaning of Care.
“If you take one piece out of the entire puzzle of the hospital, it just doesn’t run correctly,” Schaer said. “Every piece has to be there in order to make this hospital be as great as it is. And I think we know that. Each team knows that.”
More Resources
- Read about more unsung heroes of the COVID-19 pandemic: language interpreters.
- Learn more about Methodist’s COVID-19 response and get community vaccination updates.
- Read more inspiring stories about Methodist patients and staff.
- Read the latest information and articles related to COVID-19.


