
The Meaning of Care Magazine
Her Port in the Storm: Patient Leans on Methodist Doctor Through Unknowns of Long COVID
Published: Aug. 24, 2021The following is one of several profiles featuring Methodist patients who are living with the effects of long COVID – a range of health challenges that some people experience after the acute phase of COVID-19 illness. Read more long COVID patient stories:
- ‘This Story Needs To Be Told’: Omaha Woman Opens Up About Long COVID Struggles in Hopes of Helping Others
- Long COVID Patient Relies on His Faith and Methodist Doctor
- ‘Such a Fighter’: Iowa Mom Determined To Regain Her ‘Normal’ Life After COVID-19

The reminders are everywhere. Literal, tangible reminders.
Melony Stillman-Clark has sticky notes all over her Fremont home. There’s a 3-foot dry erase board in the kitchen with dates and times of appointments, school events and more. She has another small board on the refrigerator. She jots notes in her hairstyling appointment book, and she texts herself that same information to keep it fresh in her mind.
“And I still forget things,” the 42-year-old mother of two said. “I left my house the other day and drove my son halfway across town before he reminded me I was going the wrong way. Which was kind of scary.”
Melony’s brain fog is an ever-present reminder of how dramatically her life has changed since the COVID-19 pandemic began. It’s also just one of the common symptoms of long COVID – the term for a range of health challenges she and so many others have battled months after the acute phase of the illness.

COVID-19 on the Attack
“When I was in med school, we were told that we would definitely deal with a pandemic during our career,” said Misty Janssen, MD, a Methodist Physicians Clinic family medicine provider. “We all knew something like this would happen. And sadly, it won’t be the last because it’s such a global community.”
Melony actually fought COVID-19 twice last year. Before her first bout, she had been seeing Dr. Janssen for 14 years, and together they managed Melony’s Crohn’s disease, mild anxiety and depression, and occasional migraine and sinus issues.
Melony and her then-fiance, Jeff Clark, came down with COVID-19 in May 2020. The couple experienced serious but manageable symptoms – headaches, fatigue, chills, dizziness and nausea – and recovered. But Melony’s sinus problems intensified a month later with infections, pressure in her chest and headaches that kept her from working. A sinus surgery in November brought little relief.
Was COVID-19 to blame? Dr. Janssen said it’s possible, but “there’s no way to test that theory.”
Whatever the cause, the Clarks’ challenges were just beginning. In December, four months after their wedding, Jeff was hospitalized with blood clots in his lungs – likely an aftereffect of COVID-19. He was prescribed an inhaler and blood thinners, possibly for life. Soon after, Melony contracted COVID-19 a second time, and she began leaning on Dr. Janssen more than ever.

A Quarterback for Her Care
Melony was at work when she felt those familiar COVID-19 symptoms: the headaches, body aches and chills. A test confirmed what she had suspected.
“That time was horrible,” she said. “I ended up in the ER and thought I was going to die.”
With Melony in quarantine after returning home, Dr. Janssen did all she could to support her longtime patient with video checkups, a meeting at Methodist’s COVID-19 respiratory clinic in Fremont and arranging a bamlanivimab treatment with the goal of preventing her disease from progressing.
Melony weathered the storm again, but now there were much darker skies on the horizon. This time, COVID-19 left her with an array of frustrating, unexplained ailments. In the months since, she’s developed tachycardia, hyperthyroidism, fibromyalgia, chronic fatigue, insomnia, sciatica, and numbness and tingling in her legs. Her sinus issues have continued with chronic congestion, her migraines are more frequent and intense, her senses of taste and smell are impaired, and her anxiety and depression have been heightened. Her lung function has also weakened – “I feel like I have an elephant sitting on my chest,” she said.
Through it all, Dr. Janssen has been the quarterback for Melony’s care. That’s meant frequent office visits, calls and messages over Methodist’s patient portal, Methodist My Care, as well as referrals to Methodist specialists when necessary. Melony has regularly seen Ami Jones, PA-C, for cardiology; Paige Pioppi, MSN, AGACNP-C, for pulmonology; and Manjula Tella, MD, for neurology.
Their challenge in caring for long COVID patients like Melony is twofold: treating her symptoms to improve her quality of life while unraveling the mysteries of a condition unknown to doctors before last year.
“She was not somebody that I saw often in the office with complaints, so this is definitely all new,” Dr. Janssen said. “One thing that connects her symptoms is the lack of finding other conditions to explain them. All of the specialists have been in agreement that the symptoms she has seen each of us for likely tie in to long COVID.”

Uncertain Future
Melony’s parade of unexplained symptoms has turned her life upside down.
“I’m only 42, and my medicine basket now? I think I take about 18 pills a night,” she said. “It’s affected my life. It’s affected my kids’ lives. It’s affected my clients. Day by day I wake up, and if today’s a good day, I can work. And if today’s a bad day, I have to text my clients and reschedule.”
She added: “Just simple things like going on a walk with my daughter and our dogs. She walks triple the pace that I do now because I just can’t walk as fast. My kids have adjusted to the days when I’m super fatigued and I have a migraine. They’ve adjusted to, ‘We have to leave Mom alone today. She’s having a bad day.’ I can’t enjoy my life with my kids.”
The most difficult parts of long COVID, Melony said, are the unknowns – about her long-term prognosis, how to treat her brain fog and if she’ll ever be the wife and mother she wants to be again.
“I feel like I’m the same as I was six months ago. I don’t know that I feel any better,” she said. “I feel like if anything, the brain fog is getting worse. It’s really hard because they can treat the physical part of it, but the mental part of it … I feel like I have dementia. That part is so frustrating, debilitating and exhausting.”
Jeff’s commitment to Melony is as strong as ever, but he can’t help but wonder what the future holds.
“No matter how somebody says it, it’s going to sound wrong, but the woman I fell in love with is not the woman I’m in love with today,” he said. “She has changed so much with the brain fog, tachycardia, her mental issues, and her overall physical health. She’s not the woman I fell in love with, but she’s the woman I’m I love with today. Will I ever get that woman back? I don’t know. Time will tell.”
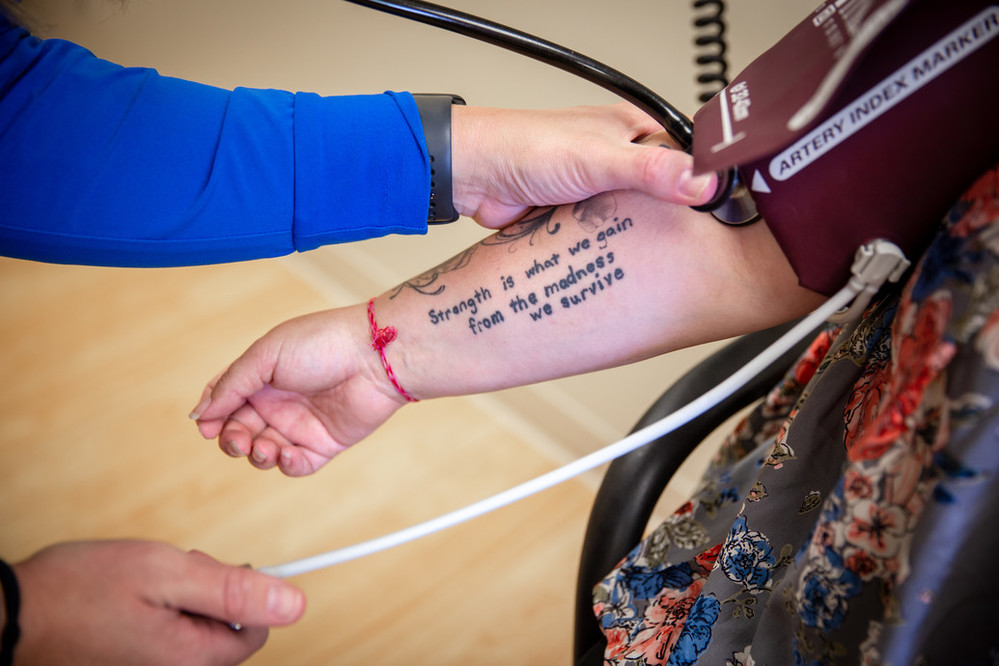
“She Will Continue To Fight”
Melony chose to share her story not for sympathy, but to make people aware of how COVID-19 can affect someone long after they’re first sick.
“I just want people to know that this is a real thing,” she said. “Just because I had it and I survived doesn’t mean that my life hasn’t changed because of it. It has affected our lives tremendously.”
When she looks back on all she’s been through, she immediately thinks of her support system.
She’s grateful to her clients for their flexibility, for bringing food to her home, for mailing checks during the initial COVID-19 shutdown and “just texting me to ask if they can do anything.”
She’s thankful for her husband for his support and patience, even as he’s battled his own COVID-related challenges.
Said Jeff: “We refer to each other as our persons, meaning that we finally found the person that we know we’re going to spend the rest of our life with. We found that person in our life that makes us feel comfortable, gives us the drive, gives us the hope and is a support system.”
And she applauds Dr. Janssen for her devoted care, even when there have been far more questions than answers.
“It means a ton to me because I know that she actually does care about me and my well-being,” Melony said. “If you’ve never met her, it’s hard to explain, but she really is a genuine, caring person.”
Together, they’ll continue to navigate Melony’s challenges in hopes of getting her back to the life she dreams of.
“I have admired her attitude the whole time,” Dr. Janssen said. “Each time she comes in, she’s had some fairly devastating or some impactful symptoms. But she’s always ready to move forward and very willing to do anything she can to improve her health and feel better. She has not given up by any means, and she will continue to fight.”
Photos and video by Daniel Johnson
More Resources
- Read more from the summer 2021 issue of The Meaning of Care Magazine.
- Read more Methodist updates about COVID-19.
- Follow Methodist on Facebook, Twitter and Instagram.


