
The Meaning of Care Magazine
‘Such a Fighter’: Iowa Mom Determined To Regain Her ‘Normal’ Life After COVID-19
Published: Aug. 24, 2021

The following is one of several profiles featuring Methodist patients who are living with the effects of long COVID – a range of health challenges that some people experience after the acute phase of COVID-19 illness. Read more long COVID patient stories:
- ‘This Story Needs To Be Told’: Omaha Woman Opens Up About Long COVID Struggles in Hopes of Helping Others
- Long COVID Patient Relies on His Faith and Methodist Doctor
- Her Port in the Storm: Patient Leans on Methodist Doctor Through Unknowns of Long COVID
After fighting for her life last winter, Sarah Drummond spent the spring learning how to live again.
Sarah, 36, was one of the millions of Americans who developed COVID-19. After she became ill in November, her condition quickly deteriorated. The Atlantic, Iowa, woman tested positive on a Friday and was coughing up blood clots the following Monday, she said. She was taken to Methodist Jennie Edmundson Hospital’s Critical Care Unit, where she was intubated and in a coma – “a black hole,” she said – for over five weeks.
She didn’t know the battle that awaited her when she regained consciousness. But her thoughts immediately went to her 17-month-old, Aiden.
“He’s my whole inspiration,” she said. “I knew right then and there that I was going to fight to get back to him.”

An Unexpected Decline
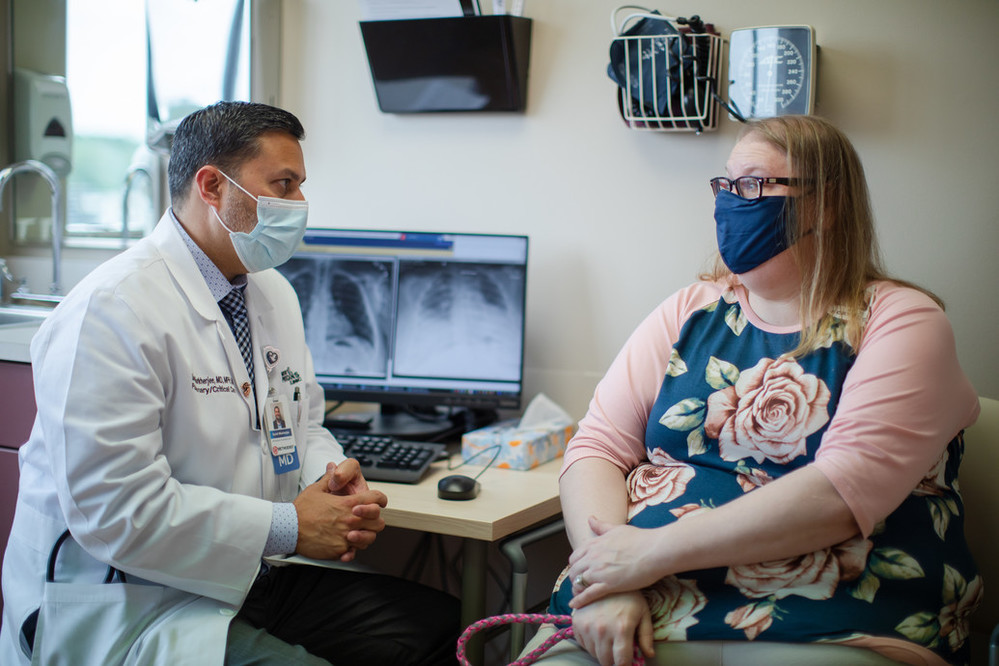
Pulmonologist Sumit Mukherjee, MD, who also specializes in critical care, has cared for numerous COVID-19 patients at Jennie Edmundson with inspiring and heartbreaking outcomes. Sarah’s case stood out for him from the beginning.
“This was really unexpected for her and her family,” he said, noting her age and health – she had put on weight after the birth of her son but had no other medical conditions.
An especially difficult moment came as Sarah, now on a ventilator, continued to show signs of decline.
“I hadn’t taken care of anybody with COVID-19 who had a child that young, and I did think we were going to lose Sarah,” said Dr. Mukherjee, a father himself. “There were several days that we were certain she wasn’t going to survive. I remember having that conversation with her husband, and I could hear her son in the background crying. He was crying for his mom. It was heartbreaking to hear.”
Sarah remembers none of it.
Then, “all of a sudden, I woke up.”
Long Road Back
Looking back, Sarah describes herself as a vegetable. Her body had been weakened by COVID-19, weeks of inactivity and powerful drugs – paralytics – used to help her ventilator do its work.
But she was alive.
Sarah was transferred to Madonna Rehabilitation Hospital in Omaha, unable to walk, hold a fork or do much of anything for herself. Her son also wasn’t allowed inside the facility. Staff estimated she may have needed up to 12 weeks of occupational and physical therapy. Sarah had other plans.
“I said, ‘You’ve got 30 days.’
“They looked at me and said, ‘How much therapy are you wanting a day?’
“I said, ‘How long are your therapists here? Because I don’t care. I’m going home in 30 days.’”
She didn’t quite meet her ambitious goal, but it still paid dividends. After six weeks of rigorous therapy to build muscle and relearn skills most people take for granted, Sarah was ready to leave Madonna. For her hard work and positive attitude, she was given Madonna’s Spirit Award.
“She is such a fighter,” Dr. Mukherjee said. “They were so inspired by her at Madonna. She was pushing them, and, boy, as far as recovery goes, that means so much.”
But Sarah had a bigger reward waiting.
On March 12, with the aid of a walker, she stepped out of Madonna and embraced her husband, Lee, and 20-month-old Aiden. It was the first time she had held her son since November.
“I walked out that door and grabbed my baby, and that was the best thing ever,” she said.
Sarah was headed home, but she wasn’t out of the woods.

New Challenges Emerge
A postmaster with the U.S. Postal Service, Sarah was determined to return to work. Achieving that goal was months away. She still faced significant physical and occupational therapy at nearby Cass County Memorial Hospital in Atlantic. For example:
“My therapist said that when I got there, my grip strength was only what a 90-year-old lady would have,” she said shortly after graduating from occupational therapy in May. “Now it’s what someone my age should have.”
And there are other unexplained ailments. Like many people experiencing long COVID, Sarah is dealing with brain fog and other mental issues – “full-blown PTSD,” as she describes it. She’s also developed diabetes.
In addition to seeing Methodist neurology and endocrinology experts, help has come from an unlikely place.
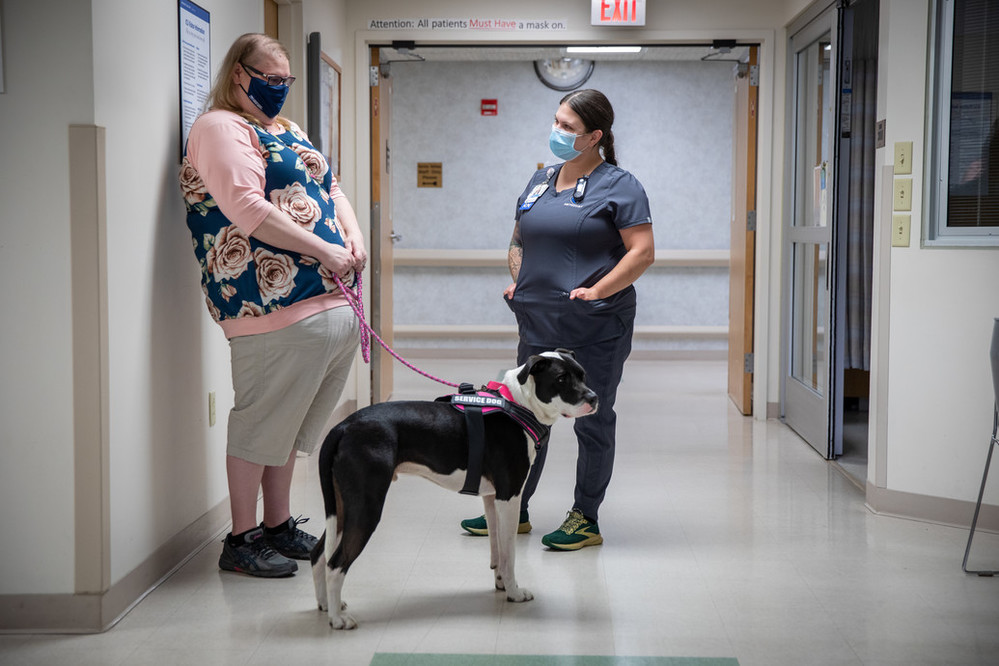
Before Sarah’s ordeal, the family dog, Bandit, wanted nothing to do with her. But since she returned home, he’s become her companion. The former “kennel mutt” is now a service animal, sensing and alerting Sarah to blood sugar issues and lying with her to calm her night terrors.
“There are times when I can have a full-on panic attack simply because I don’t want to be put in the same situation again,” she said. “I really don’t want to put my family through that again.”
She also developed atrial fibrillation in the wake of COVID-19, and she’s had issues with diminished lung function – leading to follow-up visits with Dr. Mukherjee.
“My mind and body are ready to go, but my lungs just are not keeping up,” she said in April. “I keep getting out of breath, but I just keep pushing through that.”
Her Point Person
Long COVID isn’t only affecting people like Sarah, who had harrowing experiences with COVID-19. Dr. Mukherjee has many patients who were never hospitalized but struggled with symptoms long after their infections.
“A lot of folks with COVID-19 either came to the doctor or went to the emergency room and were sent home. And after that time, they just never felt like they were the same,” Dr. Mukherjee said, noting common symptoms including fatigue, brain fog and lung issues. “There’s kind of this constellation of symptoms coming together for a lot of these folks and lasts for several months. I’ve gotten used to telling my patients that this is a long haul.”
From Sarah’s bedside at Jennie Edmundson to her recovery at home, Dr. Mukherjee has been a constant. He said he’s been inspired by how she’s pushed herself and brings out the best in her providers.
He's naturally taken the lead on her pulmonology issues. But with his compassionate approach and experience caring for COVID-19 patients, Sarah has also come to rely on him as the point person for all of her care.
“I’m not a number to him. I’m a person. And he treats me with the utmost respect,” Sarah said. “Dr. Mukherjee has set me up with probably the best team that I could ask for.”
“One Step Closer”
As the spring progressed, so did Sarah. In addition to her physical and occupational therapy, she’d walk as much as she could – first with a walker, and then a cane – building up to a few miles a day. She’d also take Bandit to the dog park, where she knew the ground was uneven so she could improve her balance.
Her hard work was paying off, and she returned to her job – now with Bandit by her side – in early May for two hours a day, five days a week.
Meanwhile, she was set on achieving another goal at her next checkup with Dr. Mukherjee.
“I’m walking in there with no cane, no walker, no wheelchair,” she said. “Just myself and my two legs.”
On May 19, she did just that, arriving with Bandit – but no cane – for her appointment. Dr. Mukherjee was surprised and excited by her progress. He took Sarah off some medications and authorized her to up her shifts at work to four hours per day.
“One step closer to my ‘normal’ life!!!!” Sarah wrote on Facebook that evening.
“I’m Here for a Reason”
Sarah’s improvement has only continued. She started working six hours a day in June and recently returned to her normal eight-hour shifts. She’s also graduated from physical therapy.
She knows there’s still a potentially rocky road ahead. Even as her mobility and strength improve, there are long-term questions about her lung issues, diabetes and mental challenges. But she tries to have a sense of humor about what she’s been through.
When an old friend asked her this spring where she’d been, Sarah offered a deadpan reply: “In a coma.”
“We can laugh about that stuff now,” Sarah said. “That’s not a response you get every day.”
When asked what she attributes her recovery to, she doesn’t hesitate.
“My drive and motivation of having a normal life with my family,” she said. “And Dr. Mukherjee not giving up on me and fighting with me.”
As Sarah’s recovery continues, she’s making new plans – to spend time with her family, and to use her story to inspire others impacted by COVID-19.
“It could have been a death sentence,” she said. “But I’m here for a reason.”
Photos and video by Daniel Johnson
More Resources
- Read more from the summer 2021 issue of The Meaning of Care Magazine.
- Read more Methodist updates about COVID-19.
- Follow Methodist on Facebook, Twitter and Instagram.


