
Inspiring Stories
A Community in Crisis: How Methodist Responded in the Earliest Days of the Pandemic
Published: March 25, 2021

Today, with widely available COVID-19 testing and a vaccination rollout that’s making its way through the population, it can be hard to remember the anxiety, fear and lack of resources in the early days of the COVID-19 pandemic. By the time Nebraska’s first confirmed COVID-positive patient was being treated at Methodist Hospital on March 6, 2020, testing was scarce and difficult to obtain.
Methodist Health System saw a need for screening and testing, and it quickly took action. By March 8, the information technology (IT) department had operationalized the Methodist Coronavirus Hotline to screen for symptomatic patients, and Methodist Physicians Clinic had established its first COVID-19 testing site. As the virus spread and anxiety increased, dedicated respiratory clinics and a mental health support line soon followed, demonstrating Methodist’s commitment to fighting all aspects of the pandemic.
A COVID-19 Screening Tool for the Community
With a goal of preventing emergency departments (EDs) and clinics from being overwhelmed by people who suspected they had COVID-19, Methodist was the first area health system to establish a dedicated screening hotline – open to everyone in the community regardless of whether they were a Methodist patient.
Kent Sona, Methodist’s vice president of IT and chief information officer, and his team worked quickly after the events of March 6 to get the hotline up and running.
“Methodist could have sat back and not done anything with the hotline and just waited for someone else,” Sona said. “Not only did we stand it up, but we staffed it and ran the schedules. You saw teamwork and collaboration all over the place, which says a lot about our culture. I was glad IT was able to do our part.”

Methodist HealthWest recovery nurse Sue Sprinkel, BSN, RN, was one of the employees who staffed the hotline early on – an opportunity to work when Methodist limited clinic operations out of an abundance of caution. When people called the hotline, Sprinkel and her colleagues would use a screening tool to identify whether they qualified for testing.
The work could be frustrating – information changed constantly as more was learned about COVID-19, and testing continued to be scarce. Sprinkel remembered having to tell anxious families that they didn’t qualify for testing just because someone was positive in their household. Because of how limited tests were, they’d have to wait until they started showing symptoms, too.
“That was the hard part,” Sprinkel said. “We’d tell them to make sure to wear a mask, stay away from people and wash your hands. Just the basic stuff. Then we’d get a call a week or two later and somebody else had it – same family.”
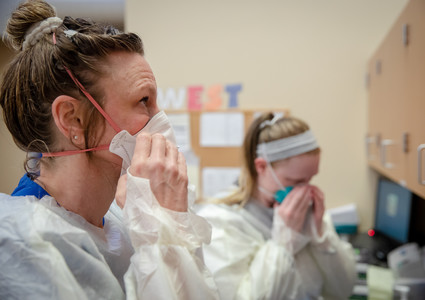
New Ways to Care
Those who did qualify for COVID-19 testing were sent to a Methodist Physicians Clinic testing site. The northwest Omaha location was chosen first for logistical and safety reasons – the staff could be moved more easily to another clinic, and the building had a separate entrance for patients who needed to be tested for COVID-19. Within two weeks, Methodist Physicians Clinic transitioned to more efficient drive-thru testing, and sites in Council Bluffs and Fremont followed.
The northwest Omaha clinic that served as the first site for the system also became the first respiratory clinic on April 1.
“We kept hearing that patients weren’t able to get seen in the clinics – patients with the flu, with sinus infections,” said Kemla Prathan, MSN, RN, performance improvement manager for Methodist Physicians Clinic.
Dedicated respiratory clinics were a solution to care for patients with respiratory and/or COVID-19 symptoms while ensuring the safety of staff and patients at other Methodist Physician Clinic locations. The health system also began utilizing telehealth in way it never had before.
“No matter what, we wanted to make sure we weren’t saying no to patients,” Prathan said. “It may not be that we could see them in the office, but there were other opportunities to get them the care they needed.”
Eventually Methodist’s urgent care locations would treat those with respiratory symptoms, and COVID-19 testing through Methodist would expand to seven trailers located outside clinics. But those early days and weeks were fast-paced and at times chaotic – a true test of communication and outside-the-box thinking.
“I was so impressed by how quickly we were able to respond and get things in place,” Prathan said. “We had so many people willing to do whatever it was – work weekends, work late hours, step out of their normal role. We had everybody offering and helping with whatever they could.”
A Mental Health Resource
That desire to step in and fill a need was also the driving force behind the Methodist Emotional Support Line – (402) 815-8255 (TALK). The community mental health resource was the brainchild of Jean Faber, corporate director of the Best Care Employee Assistance Program and the Methodist Community Counseling Program, and Tracy Madden-McMahon, president and chief executive officer of Methodist Hospital Foundation. Launched on March 30 after more quick work by the IT team, the support line is staffed by counselors from the Methodist Community Counseling Program. It continues to help those seeking guidance for mental health issues, many of which were brought on by the pandemic.

“When the world changes overnight, it comes with fear, anxiety and isolation,” Madden-McMahon said. “Suddenly our counselors were no longer able to be in schools or community sites. We saw an opportunity to share their skills in a different way.”
The list of issues people call about includes: anxiety, depression, uncertainty, fear, anger, illness, social unrest, political unrest, financial insecurity, food insecurity, struggles with remote learning, domestic abuse, substance abuse, loneliness, social isolation, suicide and grief.
“Our counselors listen,” Faber said. “They validate the person’s struggles and emotions and can refer them to resources. We encourage them to get back to seeing their counselor or consider starting counseling. Not everyone needs that additional support, but quite a few do.”
“Thanks to our generous donors, we’re able to offer this support free of charge,” Madden-McMahon said. “I’m proud that as a community, we’re changing the conversation about asking for help. It’s a sign of strength – not weakness.”
Lessons Learned
By the end of May, the Methodist Coronavirus Hotline was phased out as clinics resumed normal operations and began screening their own patients for COVID-19. Sprinkel was eager to return to her role at Methodist HealthWest but was proud of the work she did on the hotline.
“I think it was a good resource tool for people,” she said. “We helped people not run to the ED and helped calm their nerves. A lot of them were pretty anxious. We didn’t have all the answers. And we would tell them – this is what we know so far.”
Sona said that in nearly two months, 6,290 people screened negative via the hotline – preventing a significant number of unnecessary visits to the EDs and clinics. He was proud of what his team was able to contribute to the health system and community in a time of crisis.
“I always tell my staff: ‘Calm breeds calm. Panic breeds panic. Let’s stay calm. Let’s do what we can to help the business,’” he said. “You can’t be afraid to step up and take it on even if it’s not something you normally do. That’s how you make a difference in times like this.”
Prathan predicts that some of the adaptations the health system had to make during the past year are here to stay, such as an increased use of telehealth and the successful drive-thru flu shot clinics last fall.
“COVID really forced us to look at how we can provide patient care in a different way,” Prathan said. “We don’t have to continue to do things the way they have been done in the past.”
Photos by Daniel Johnson
More Resources
- Read about the unsung heroes of Incident Command who responded to the call in a time of crisis.
- Get answers to common questions about life after COVID-19 vaccination.
- Read more stories and updates on the COVID-19 pandemic.


