The Meaning of Care Magazine
‘This Story Needs To Be Told’: Omaha Woman Opens Up About Long COVID Struggles in Hopes of Helping Others
Published: Aug. 24, 2021The following is one of several profiles featuring Methodist patients who are living with the effects of long COVID – a range of health challenges that some people experience after the acute phase of COVID-19 illness. Read more long COVID patient stories:
- Long COVID Patient Relies on His Faith and Methodist Doctor
- Her Port in the Storm: Patient Leans on Methodist Doctor Through Unknowns of Long COVID
- ‘Such a Fighter’: Iowa Mom Determined To Regain Her ‘Normal’ Life After COVID-19
Becca Cook, 40, is no stranger to the pain and struggle of recovering from a life-changing medical event.
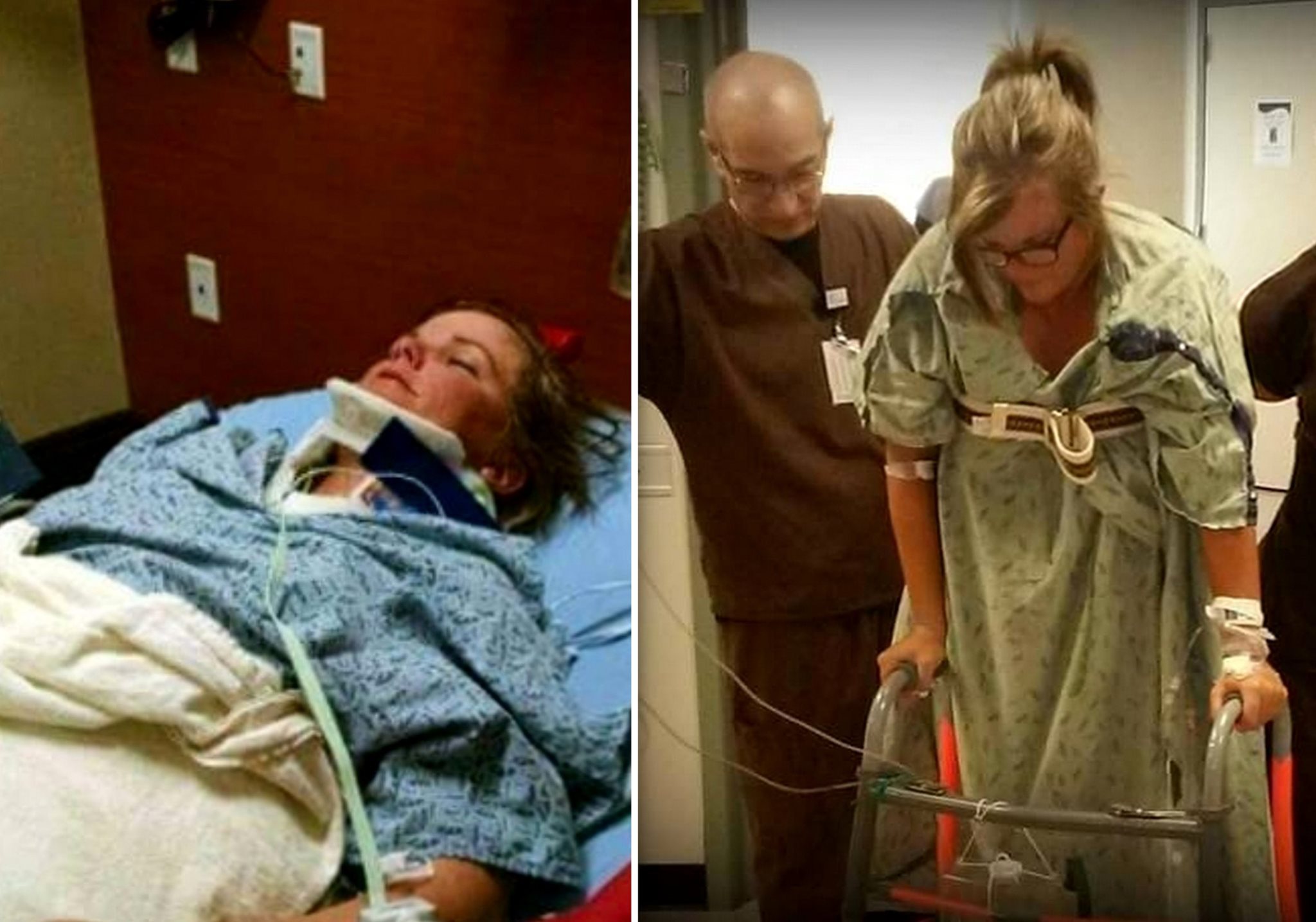
In 2015, while stuck in Arizona freeway traffic, Becca’s car was rear-ended by a pickup truck – the driver had been texting. She suffered injuries including a serious concussion and significant damage to a spinal disc and a knee.
A “horrific” two and a half years followed, with doctors’ appointments, surgeries and therapy.

“I remember them telling me, ‘Your nerve damage is permanent. You’re likely to have a permanent limp. The odds of you doing some of the things you love are slim to none,’” Becca said. “But I always believed that I would recover. It was a matter of being disabled or not disabled, and I wasn’t ready to accept that I wasn’t going to be able to live like a normal 30-something. So I just didn’t. I’m very fortunate because the odds were not in my favor.”
Becca slowly recovered, and although a final surgery left her with two orthopedic screws in her tibia, she had hope of living a somewhat normal life again. She climbed her favorite mountain in June 2018, and she moved back to her home state of Nebraska in 2019 to spend more time with her brother, sister and five nieces.
Then, in November 2020, she became ill with COVID-19. What’s followed has been “unlike any experience I’ve ever had,” she said.
COVID-19 Brings Surprise Symptom: Pain
As an asthmatic, Becca was at high risk for complications if infected with COVID-19.
“It started out kind of slow, and then all of a sudden it wasn’t slow,” she said. “I was very, very sick for 15 days, to the point that it was all very hazy. I was doing breathing treatments at home. To be honest, it was terrifying because I was struggling to breathe.”
Looking back, Becca said she expected to have lung issues, but not the pain she experienced.
“Not aches, but downright pain,” she said. “Nerve, joint and muscle pain.”

Quarantined at home but not sick enough to be hospitalized, Becca leaned hard on her primary care provider, Shane Stephenson, MD, a family medicine provider with Methodist Physicians Clinic. They exchanged updates through messages in Methodist’s patient portal, Methodist My Care, and had several virtual appointments using video technology.
Dr. Stephenson said those tools are invaluable when caring for patients in quarantine during the acute phase of COVID-19.
“Sometimes all they really needed to do was talk about what their symptoms were,” he said of virtual visits. “This offers a way to reassure them and guide them – ‘Yes, you’re safe to stay at home. These are the things I’d watch for. These things are positive and encouraging to me.’ I find those things really helpful, and – just from a patient’s mindset – very beneficial, too.”
After two weeks of isolation, Becca was cleared to leave her home and finally felt well enough to. But Dr. Stephenson made it clear that it may take some time for her to fully recover.
“My Body Was Going Haywire”
As the new year began, Becca was still struggling, but something had changed.
“I no longer felt like I was in the remnants of the acute phase,” she said. “But my body – things weren’t right. It felt like my body was going haywire.”
Her nerve, joint and muscle pain persisted, but they were joined by a cascade of new symptoms – many associated with long COVID.
She battled fatigue, brain fog, headaches, fevers, a persistent cough and bouts of dizziness. An upset stomach led to a decreased appetite, and she lost 30 pounds over the winter and spring. She began suffering from insomnia. Her legs would develop bruising with no explanation, and she began experiencing neuralgia – sharp pain in her face.
“There’s a lot of weird things,” Becca said. “There’s really not a lot of explanation of what is happening. I tell people that it’s like a new surprise every day. It’s like the gift that keeps on frickin’ giving.”
Dr. Stephenson is just as frustrated.
“You see them and hear their story, but we just don’t have a lot of things in our tool belt to help,” he said. “And there really doesn’t seem to be any rhyme or reason in regard to who’s getting long COVID versus who’s not. This coronavirus has a wide breadth of activity in the body, and we’re probably still only scratching the surface of everything that it’s responsible for and can cause.”
But he also sees momentum with research, vaccines and treatment that will only continue. And he finds it as rewarding as ever to care for his patients.
“I sometimes tell them that I’m going through this for the first time,” he said. “There’s a lot we don’t know about it. But here’s what we do know. And I’m going to be here with you through it.”

Progress, Then Setbacks
With Dr. Stephenson managing her care plan, Becca has seen a pulmonologist, physiatrist, neurologist and rheumatologist.
Her recovery has been slow and uneven. At times, her progress is overshadowed by new setbacks.
For example, in early May she thought her neuralgia was under control. Then, “for no reason, it’s back,” she said.
Long COVID also rekindled issues from her 2015 accident. She’d had no problems with the screws in her tibia after her surgery. But that area was so frequently painful and irritated this year that she flew back to Arizona in June to have them removed.
In fact, pain throughout Becca’s body has been a constant during her recovery. She considers herself to have a high tolerance, but she continues to be surprised.
“The level of pain has been shocking, and the lingering pain has been shocking,” she said.
Dr. Stephenson and other specialists are able to treat Becca’s symptoms, but the causes of many are a mystery. He wonders if Becca had a tendency toward an autoimmune disorder that COVID-19 ignited. But it’s nothing her team of doctors have been able to diagnose.
“It seems to me that COVID-19 has kind of triggered a cascade of multisystem inflammation,” Dr. Stephenson said. “That has hit her pretty hard.”
Becca puts it more bluntly: “From an orthopedic and neurological standpoint, I feel like COVID-19 took a torch to every issue I ever had and lit it on fire.”
Despite the challenges and unknowns, Dr. Stephenson has a positive outlook about Becca’s recovery.
“She does seem to have one thing after another, but I think there have been a lot of small victories along the way,” he said. “I’m still optimistic that we see her get all the way back to herself and back to living life.”
Continuing Isolation
The intense pain and revolving door of new symptoms have been frustrating for Becca, but the hardest part of long COVID has been the isolation.
Becca enjoys being outside and golfing, but now her lungs don’t tolerate allergens well. She loves to play with her nieces and attend their sporting events, or to attend a happy hour or dinner with friends, but long COVID often alters her plans.
“Even from a social aspect, it’s different now,” she said. “It’s hard to even do that because I never really know how I’m going to feel. I have good days and bad days, but I don’t know the timing of it. It definitely has affected my social life and even my desire to be social. It takes a lot of energy.”
Even talking to other people can be isolating, she said.
“I’m fortunate that I’m not alone because I have Dr. Stephenson, who gets it. But as far as day to day, it’s an isolating feeling because people don’t get it,” she said. “Not having answers and not having a lot of people who can relate – it’s probably the worst part.”

Determined To Keep Fighting
While many people can’t relate to Becca’s long COVID journey, she knows that many people can.
“My main reason for telling this story is so that people are aware, and to maybe help someone,” she said. “Maybe it will inspire someone to go after that care, or just help someone to know they’re not crazy. This story needs to be told. It’s such an issue that is untold and under accounted for.”
As her recovery continues, Becca is focused on gratitude, staying positive and controlling what she can – an approach she adopted while recovering from the car accident.
“Regardless of your circumstances, life goes on with or without you,” she said. “You either make the choice to let it go on without you, or you do your best to keep up. So that’s what I’m doing.”
She’s grateful to have Dr. Stephenson managing her care.
“One hundred percent, he has been the most valuable asset in this,” she said. “He’s always had my back. This has been a team approach, and I never felt like I was alone with it. He will be involved in every aspect of my care for as long as I’m around.”
And she’s grateful to simply be here, still fighting and sharing her story.
“I know there are a lot of families who would give anything to have their family members still with them even if they were struggling,” she said. “I have the luxury of being alive when a lot of people don’t.”
Photos and video by Daniel Johnson
More Resources
- Read more from the summer 2021 issue of The Meaning of Care Magazine.
- Read more Methodist updates about COVID-19.
- Follow Methodist on Facebook, Twitter and Instagram.


