
The Meaning of Care Magazine
A Cut Above: Methodist’s Cardiothoracic Surgeons Build on Excellence
Published: April 21, 2021
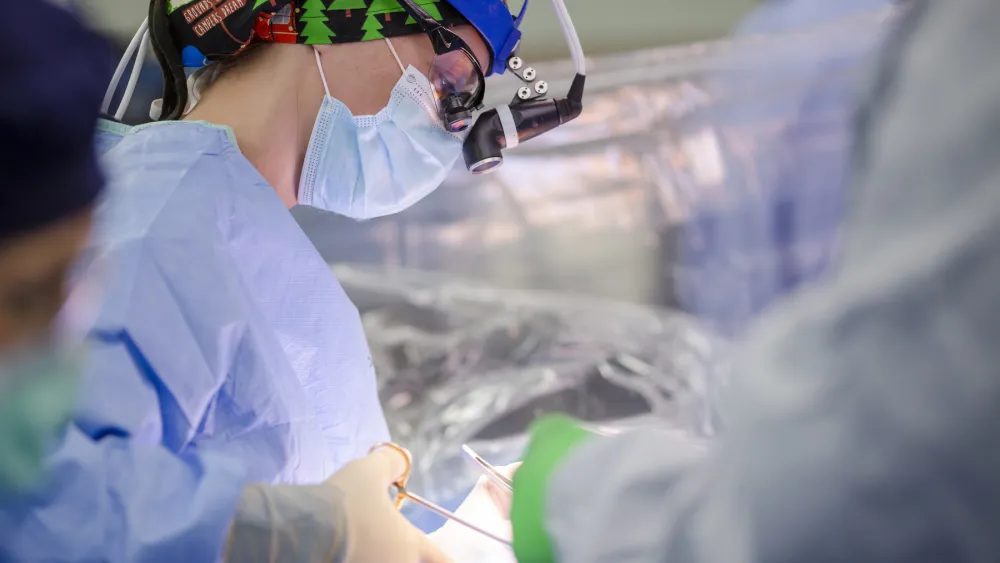
“I’m the recipient of as close to a medical miracle as you can get,” said 68-year-old Joe Johnston.
Joe and his wife, Judy, called the events of Nov. 26 their “Thanksgiving miracle.” It started with the decision to have Thanksgiving dinner at their son’s house near Methodist Hospital in Omaha instead of their home in Iowa’s Loess Hills near Mondamin. It ended with Methodist cardiothoracic surgeon HelenMari Merritt, DO, operating on Joe to repair a Type A aortic dissection – a tear in the upper aorta – only to find a dangerous hole in his aorta that was somehow being walled off by his body.
“He should be dead – 100%, he should be dead,” Dr. Merritt said.
But today Joe is thriving and back at work at the Omaha photography studio he and Judy have run for more than 35 years.
“I’m resolved to not screw this up for all the talented people who did their job and allowed me to still be vertical,” he said.
Joe’s story reminded Dr. Merritt of what attracted her to her specialty.
“I think that’s just a perfect example of what drives people to go into surgery,” she said. “Being able to be a part of that – being a part of a forever story for a family and getting a chance to make a tangible difference in someone’s life.”
Teaching Each Other
Dr. Merritt joined Methodist Physicians Clinic’s cardiothoracic surgery team in 2020. The team – which also includes John Batter, MD – performs surgeries at Methodist Hospital and sees patients at its office in Omaha and outreach locations at Methodist Jennie Edmundson Hospital and in Lincoln.

“When I came to Methodist, I was really excited about joining a team that has already had phenomenal outcomes,” said Dr. Merritt, referencing the work of Dr. Batter, who has been performing surgeries at Methodist Hospital since 1997.
Dr. Batter has dedicated the last 13 years as cardiothoracic surgery section chief to building up the program, consistently earning it a top rating from the Society of Thoracic Surgeons. He praised Dr. Merritt’s hiring and the “incredible talent and skill” she adds to the team.
“She’s very interested in minimally invasive valves, and I jokingly refer to myself as the maximally invasive valve guy,” he said.
When Dr. Merritt joined the cardiothoracic team, she brought with her a focus on minimally invasive valve repair and replacement as well as minimally invasive approaches to lung cancer reduction. She can do the sternum-breaking open-heart surgery that Joe needed. But she can also replace a patient’s valve with no more than a small incision the size of her finger, and remove cardiac masses or blood clots with a catheter.
Dr. Merritt enjoys her working relationship with her partners and the synergy between surgeons at different stages of their careers. She praised the multidisciplinary heart valve team that’s continued a successful transcatheter aortic valve replacement (TAVR) program even in a pandemic. She’s helping her partners learn some of the minimally invasive techniques she’s passionate about while Dr. Batter is helping her master a technique that has long distinguished cardiothoracic surgery at Methodist Hospital – beating-heart surgery.
Coronary artery bypass graft (CABG) surgeries are often performed by stopping the heart and using a heart-lung machine to take over the function of those organs. But in a beating-heart surgery, or off-pump CABG surgery, the heart keeps pumping blood to the body. Dr. Batter said it’s a more difficult way to perform surgery, but patients often benefit with shorter hospital stays, faster recoveries and less risk of bleeding, blood transfusions and stroke. Dr. Batter estimates that he’s performed more than 3,000 beating-heart surgeries over two decades, making Methodist Hospital a regional leader in the practice.
“When patients see the cardiothoracic surgeons at Methodist, they’re going to get great care – whether it’s a heart valve problem or a tumor in their lung,” Dr. Merritt said. “We have a collaborative approach between the surgeons here and make sure the patient gets the right incision.”
Multidisciplinary Collaboration
At Methodist, collaboration between surgeons often reaches across disciplines and leads to better patient outcomes.
Recently, Methodist’s cardiothoracic surgeons and electrophysiologists have seen success with their partnership for the convergent procedure – an innovative way to treat patients with persistent atrial fibrillation (AFib), a type of heart arrhythmia where the heart beats irregularly. Drs. Batter and Merritt began performing the procedure at Methodist Hospital in early 2020, and it’s now the only hospital in the state to offer it. In just over a year, Methodist has become a top five program out of 225 in the country based on volume – demonstrating the skill of the physicians and demand for the treatment.
“You don’t have to live forever with AFib and blood thinners. We’ve got a plan,” Dr. Batter said. “Methodist Hospital has the most comprehensive program and experienced doctors in the whole state doing this.”
Whereas a traditional ablation to treat AFib only ablates – or burns – the tissue surrounding the pulmonary veins on the inside of the heart, the convergent procedure also ablates the area of the pulmonary veins on the outside of the heart. The more scar tissue that’s created, the less electrical activity there is to trigger AFib.
The procedure for those with persistent AFib starts with a cardiothoracic surgeon surgically ablating the outside of the heart. The surgeon can also place a clip on the left atrial appendage – like a surgical version of the minimally invasive WATCHMAN™ procedure that decreases the risk of stroke in AFib patients. Six weeks later, an electrophysiologist creates a voltage map to see how much electrical activity is still present and uses a catheter to further ablate the inside of the heart and eliminate that activity.
Methodist Physicians Clinic electrophysiologist Matthew Latacha, MD, credits the teamwork between him and electrophysiologist Jeffrey Mahoney, MD, and the cardiothoracic surgeons for the rapid success of the convergent procedure at the hospital.
“I think this just highlights the cardiovascular care that Methodist Hospital has been delivering, especially in the last few years,” Dr. Latacha said. “Now we have another procedure, which is unique to us in the community, that we can offer patients who otherwise wouldn’t have many options for AFib.”
Dr. Merritt also points to the strength of multidisciplinary collaboration for the hospital’s Pulmonary Embolism Response Team (PERT) program. The developing program aims to standardize the response to patients suffering from a pulmonary embolism by bringing together a vascular surgeon, emergency medicine physician, internal medicine physician, pulmonologist and cardiothoracic surgeon to determine a patient’s options and best course of treatment in a timelier manner.
“Previously, it was a case-by-case basis, and these patients were probably treated differently depending on what physician was admitting them to the hospital,” said Methodist Hospital emergency medicine physician Joseph McCaslin, MD. “Our goal in taking care of patients the best way we can is taking out that deviation and making it standard so that everybody gets the same approach.”
Vascular surgeon John Park, MD, who’s been championing different approaches to treating pulmonary embolisms for nearly a decade, is pleased with the recent momentum of the program.
“The goal is awareness,” he said. “If you, as a physician, have a patient with a blood clot, you have to know that there are options for treatment. We can offer input.”
As recently as five years ago, the most common treatment option for someone with a pulmonary embolism was anticoagulants. Now in certain cases, Dr. Park and the vascular surgery department can perform catheter-directed thrombolysis, which uses medicine to dissolve the clot and ultrasound to fragment it. In rare circumstances a cardiothoracic surgeon is needed to remove the clot with a suction device known as AngioVac – a treatment option Methodist couldn’t offer before Dr. Merritt’s arrival.
“It’s not something that needs to be done often, but it’s not easy to do,” said hospitalist Ty Huebert, MD. “You have to have the right-skilled surgeon. She can take a person who would otherwise die and give them a chance to live.”
Counting Blessings
The commitment to excellence, the push for innovation, the multidisciplinary collaborations – it’s all for the cardiothoracic surgery team’s pursuit of giving patients their lives back so they can focus on their loved ones and passions.
“It’s really invigorating every day to wake up,” Dr. Merritt said. “We get to do so many different surgeries that impact people’s lives in different ways.”
“Our program has been developed and continues to be developed for the best patient outcomes and satisfaction,” Dr. Batter said. “We ask: What’s the best way to take care of AFib? What’s the best way to replace a valve? What’s the best way to bypass a heart?”
And sometimes the best way is what Dr. Merritt calls the “big, ugly cut” – maximally invasive surgery to save a life when the minutes are precious and the outcome is uncertain.
Joe proudly shows off the scar from his own big, ugly cut. It’s a reminder of “Papa’s amazing Thanksgiving miracle” and the compassionate, efficient and expert care that saved his life so he can celebrate next Thanksgiving with his family.
“I count my blessings,” he said. “The surgical team was available and put all the pieces together. I can only imagine how conscientious and trained that group of people is. I have nothing but the highest level of gratitude.”
Photos and video by Daniel Johnson
More Resources
- Read more from the spring 2021 issue of The Meaning of Care Magazine.
- Learn more about the minimally invasive transcatheter aortic valve replacement (TAVR) offered at Methodist.
- Learn more about the WATCHMAN™ program at Methodist Hospital, which was recently named the No. 1 program in volume out of 43 in the Upper Midwest region.
- Learn more about cardiothoracic surgery services at Methodist.
- Learn more about Tyler Kahle’s story and how his tragic death transformed care at Methodist Hospital.


