
The Meaning of Care Magazine
A Lesson in Life and Longboarding: ‘Even When You Fall, You’ve Got To Keep Going’
Published: April 10, 2023
At 30 miles per hour down a steep North Omaha hill, competitive longboarder Tosh Newton, 25, of Kansas City, Missouri, appeared to take flight as his T-shirt clung to his chest and flapped in the wind behind him.

As he gained more speed, his board began to wobble. The wheels beneath him grinded against the concrete before he slipped off and skidded across the pavement.
He bounced up to his feet and flashed a coy smile.
“That’s just what longboarding is,” he said by covering the stoma – or hole – in his neck with one finger. “You know how to fall and get back up. If you want to keep going, you have to keep going.”
And he walked up the hill to ride down it again.
A Terrifying Reality
Tosh, of Kansas City, Missouri, developed a raspy voice at a young age and assumed it was the result of adolescent vocal changes. But biopsies in 2016 revealed something more serious: papillomas – or wartlike growths – scattered up and down his vocal cords, likely from a virus he contracted early in life.
He received multiple laser excisions to remove the benign tumors, but after about a year of treatment, they turned cancerous. In 2017, he underwent a partial laryngectomy – the surgical removal of his larynx, or voice box – which took more of a toll on him than the chemotherapy and radiation that followed.
“When I woke up from surgery, the first thing I did was touch my neck,” Tosh said. “Sure enough, there was a tube there. I was stunned. I knew that now I was going to be that guy with a hole in his throat. The sick person with a robotic voice that you see in all those smoking commercials.”
Tosh, one of the strongest swimmers on his high school dive team at the time, could no longer swim with a stoma in his neck. And after several complications, he also lost the ability to eat and drink effectively. He eventually received a feeding tube in his stomach and quickly realized how much he had taken for granted.
“Something as simple as going out to eat with friends,” he said. “The waiter would always ask, ‘Do you want anything?’ All I could say was, ‘Nope, I’m OK.’”
But he wasn’t.
“I hit a really low point,” he said. “Just really depressed.”
Everywhere he went and in everything he did, it seemed, stood a harsh reminder of his new reality.
Nothing Left To Lose
2019 brought another wave of lows. Tosh developed a dysfunctional larynx, which led to a full laryngectomy and reconstructive surgery. That’s when he received a tracheoesophageal voice prosthesis (TEP), which allowed him to speak but not very well due to delayed wound healing and more serious complications.
He was hospitalized for a month.
After receiving care at some of the most reputable hospitals in the country – including Barnes-Jewish Hospital in St. Louis, Massachusetts General Hospital in Boston and The Mount Sinai Hospital in New York City – Tosh heard about a laryngectomy symposium at Methodist Estabrook Cancer Center (MECC) in Omaha.
He made the three-hour drive in November 2019 because he had nothing left to lose, he thought. But he had no idea how much he was about to gain.
Fostering Healing, Independence
Aside from inspiring and educational speakers, MECC’s symposium led Tosh to oncology nurse navigator Katie Holling, BSN, RN, OCN, who became what she calls “his go-to for any questions or needs during his survivorship journey.”
“Tosh was cured of cancer when I met him,” Holling said. “But from a survivorship standpoint, he wasn’t really living. His quality of life needed significant improvement. He was beat up from treatment, carrying all these devastating side effects with him, yet there he was at our door, ready and eager to do and try anything just to function.”
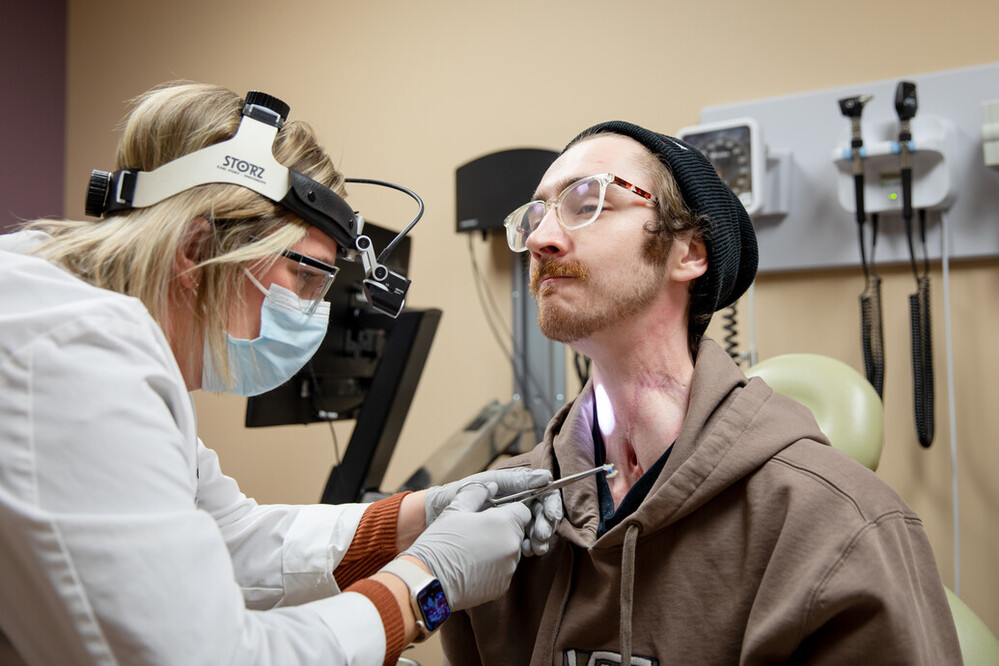
Tosh also met speech and language pathologist Carla Gress, ScD, CCC-SLP, who quickly identified the support he needed for speaking, swallowing, breathing and, perhaps most important, healing.
“I knew he needed to establish care with the right head and neck surgeon who could manage the horrible complications he was experiencing,” Gress said.
She introduced him to surgical oncologist Andrew Coughlin, MD, who eventually performed several procedures on Tosh, including dilations to stretch his patient’s esophagus, which had become thick and narrow from treatment and complication scarring.
“We were getting to the point where he was frequenting the operating room and having to go under for dilations every month or so just so he could swallow,” Dr. Coughlin said. “And for a young guy, that’s no way to live. I knew we had to think outside the box.”
Dr. Coughlin proposed the idea of self-dilations at home, where Tosh would apply a topical numbing agent to the back of his throat to prevent a gag reflex before sliding a lubricated tube down his esophagus to open it back up each time it grew tight.
“It definitely takes the right person,” Dr. Coughlin said. “It takes a lot of trust. And yes, it takes a lot of practice and hand-holding in the office initially. But Tosh is a remarkable human with a can-do nature. I knew he could do it.”
“I’m definitely a doer,” said Tosh, who also benefitted from nutrition services as part of Methodist's Harper's Hope Cancer Survivorship Program. “I always have been. Dr. Coughlin recognized that. My whole care team did. They recognized a lot of things that no other place I received care from did. They’re different. And they’ve got me for life.
“Treating People – Not Patients”
In 2020, Tosh graduated from Northwest Missouri State University. That's where he met his current girlfriend, Francesca Infranca, who's been the biggest piece of his support system for much of his survivorship journey. He currently works in technical support at a Kansas City call center, and he's become an old pro at speaking with his TEP. He performs self-dilations every other day at home and, if necessary, he can also replace his own feeding tube – something he maintains in the event that swallowing isn’t an option.
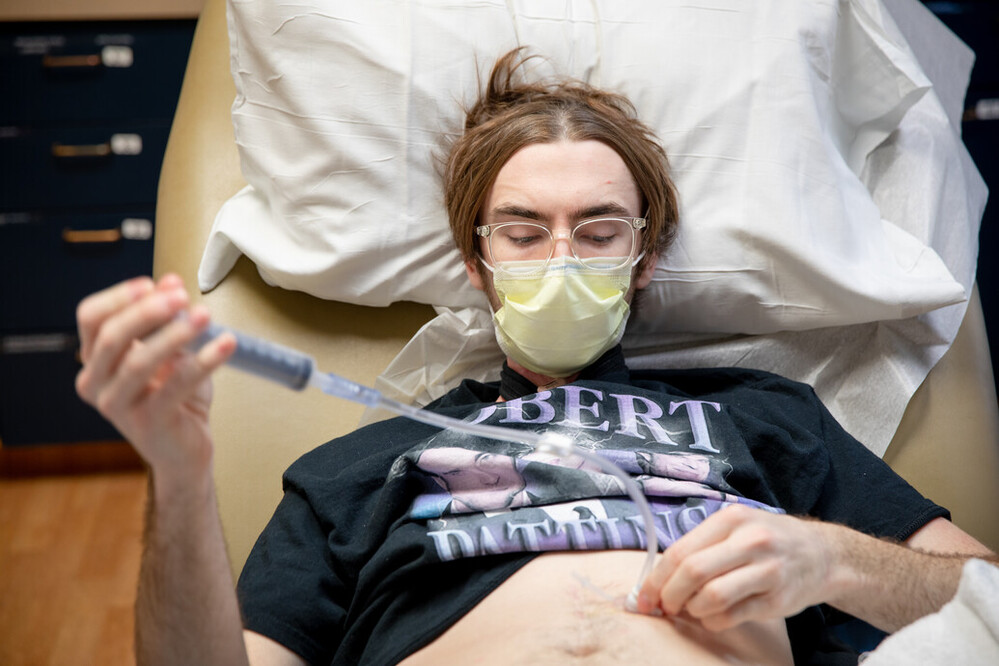
He credits his Methodist care team for helping him feel more like himself – confident and independent –and less like a patient.

“I think The Meaning of Care is just that,” Gress said. “It’s about treating people – not patients. Recognizing they’re a person, first, with desires and interests that aren’t all medical.”
Although Tosh’s interest in longboarding evolved once his days in the pool were over, he finds bittersweet irony in how well the sport suits him. Thanks to the support he’s received through Methodist, he knows each hill he’s forced to walk up means another opportunity to fly.
“Sometimes you’ve got to go through some stuff to find the good and come out better on the other end,” Tosh said. “So if you want to live, you’ve got to keep living. Even when you fall, you’ve got to keep going.”
More Resources
- Read more from the spring 2023 issue of The Meaning of Care Magazine.
- Learn more about head and neck oncology treatment at Methodist.
- Learn more about cancer rehabilitation at Methodist.
- Learn more about the Harper’s Hope Cancer Survivorship Program at Methodist.


